Living with chronic pain can feel overwhelming, especially when traditional treatments haven’t provided the relief you need. If you’re searching for radiofrequency ablation NYC options, you’re likely looking for a proven solution that can offer long-lasting pain relief without major surgery. This minimally invasive procedure has transformed the lives of countless patients struggling with persistent pain conditions.
Radiofrequency ablation (RFA) represents a significant advancement in interventional pain therapy, offering hope to those who have exhausted other treatment options. By precisely targeting the nerve pathways responsible for transmitting pain signals, this innovative procedure can provide substantial relief for months or even years.
Understanding Radiofrequency Ablation: The Science Behind Pain Relief
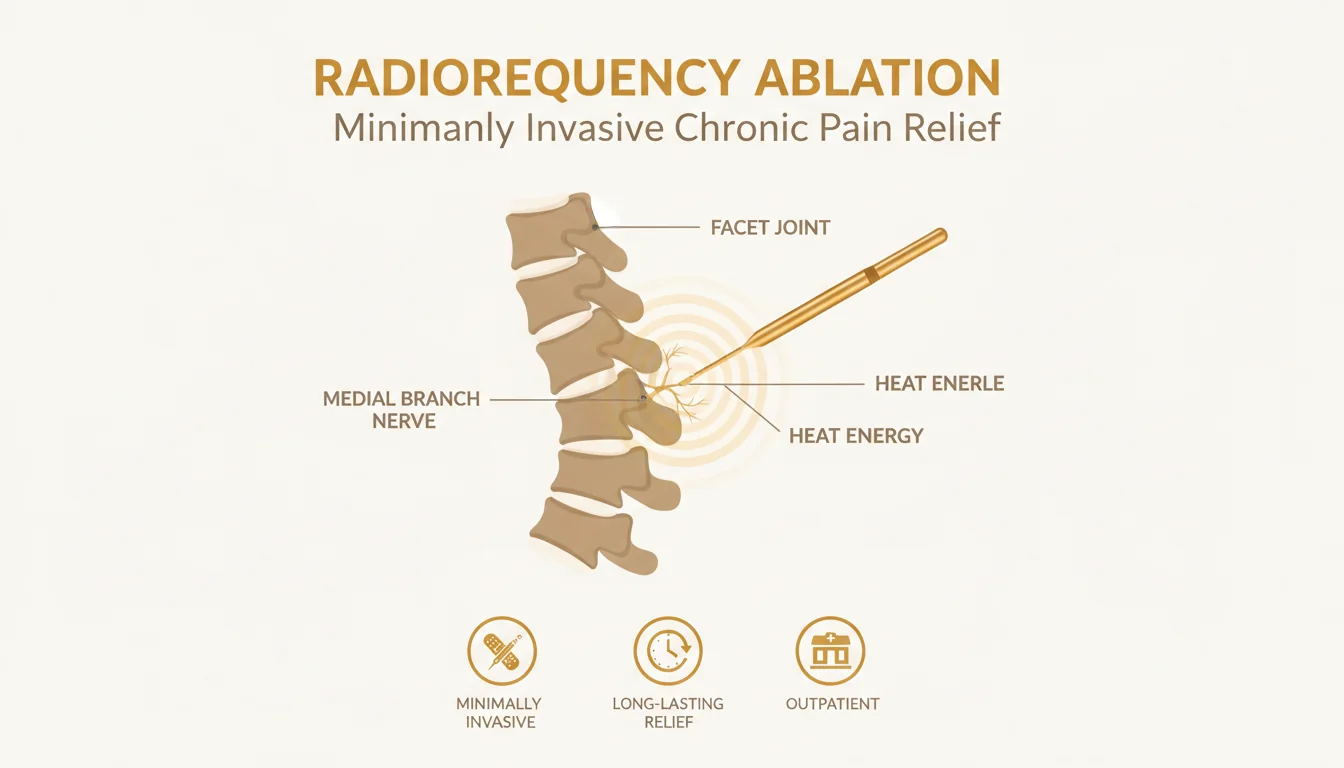
Radiofrequency ablation, also known as nerve ablation therapy, is a minimally invasive medical procedure that uses controlled heat energy to interrupt pain signals traveling along specific nerves. The technique involves inserting a thin needle-like electrode near the targeted nerve and applying radiofrequency energy to create a precise lesion that blocks pain transmission.
The procedure works by heating nerve tissue to approximately 80-90 degrees Celsius, which disrupts the nerve’s ability to send pain signals to the brain. This targeted approach allows physicians to address the source of pain without affecting surrounding healthy tissue or causing significant damage to the treated area.
What makes RFA particularly effective is its precision. Using advanced imaging guidance, such as fluoroscopy or ultrasound, pain management specialists can accurately locate the specific nerves responsible for chronic pain and treat them with remarkable accuracy.
The Technology Behind RFA
Modern radiofrequency ablation systems utilize sophisticated technology to ensure optimal outcomes. The radiofrequency generator produces electromagnetic waves at a frequency of approximately 500,000 Hz, creating controlled thermal energy that precisely targets nerve tissue.
Temperature monitoring systems built into the electrodes provide real-time feedback, ensuring the procedure remains within safe parameters while achieving therapeutic temperatures. This technological precision is what makes RFA both safe and effective for long-term pain management.
Conditions Treated with Radiofrequency Ablation NYC
Radiofrequency ablation has proven effective for treating various chronic pain conditions, particularly those involving specific nerve pathways. Understanding which conditions respond best to this treatment can help patients make informed decisions about their pain management options.
Facet Joint Pain
Facet joint ablation is one of the most common applications of RFA. The facet joints, located along the spine, can become sources of chronic pain due to arthritis, injury, or degenerative changes. When these joints become inflamed or damaged, they can cause persistent back pain and neck pain that significantly impacts daily activities.
RFA targets the medial branch nerves that supply sensation to these joints, effectively interrupting the pain signals without affecting motor function or other important nerve pathways.
Sacroiliac Joint Dysfunction
The sacroiliac joints, located where the spine meets the pelvis, can be another source of chronic lower back pain. When conservative treatments fail to provide adequate relief, radiofrequency ablation can target the lateral branch nerves that innervate these joints.
Patients with sacroiliac joint dysfunction often experience pain that radiates into the buttocks, hips, or legs. RFA can provide significant improvement in these symptoms when performed by experienced practitioners.
Other Pain Conditions
Beyond spinal conditions, RFA can be effective for treating:
- Chronic knee pain from osteoarthritis
- Occipital neuralgia and certain types of headaches
- Trigeminal neuralgia
- Peripheral nerve pain syndromes
- Certain types of cancer-related pain
The RFA Procedure: What to Expect
Understanding the RFA procedure process can help alleviate anxiety and ensure patients are well-prepared for treatment. The entire procedure typically takes 30-90 minutes, depending on the number of nerves being treated and the specific technique used.
Pre-Procedure Preparation
Before undergoing radiofrequency ablation, patients typically undergo a comprehensive evaluation, including a detailed medical history, physical examination, and often diagnostic nerve blocks to confirm that the targeted nerves are indeed the source of pain.
Patients may need to temporarily discontinue certain medications, particularly blood thinners, and arrange for transportation home after the procedure, as mild sedation is often used for comfort.
During the Procedure
The RFA procedure is performed in an outpatient setting, often in a specialized procedure suite equipped with fluoroscopy or other imaging guidance. Here’s what typically happens:
The patient lies on an examination table, and the skin over the treatment area is cleaned and sterilized. Local anesthetic is administered to numb the insertion site, ensuring patient comfort throughout the procedure.
Using imaging guidance, the physician inserts a thin radiofrequency electrode through the skin to the precise location of the target nerve. Once proper positioning is confirmed, a small electrical current is applied to test the electrode placement and ensure it’s positioned correctly.
The radiofrequency energy is then delivered for a specific duration, typically 60-90 seconds per site, creating the therapeutic lesion that interrupts pain signal transmission.
Recovery and Post-Procedure Care
Following the procedure, patients are monitored for a short period before being discharged home. Most people can resume normal activities within a few days, though heavy lifting and strenuous exercise may need to be avoided for a week or two.
Some patients experience immediate pain relief, while others may notice gradual improvement over several weeks as inflammation subsides and the full effects of the procedure become apparent.
Benefits and Effectiveness of Minimally Invasive Pain Management
Radiofrequency ablation offers numerous advantages over traditional surgical approaches and long-term medication management. Understanding these benefits can help patients appreciate why RFA has become a preferred treatment option for many chronic pain conditions.
Long-Lasting Relief
One of the most significant advantages of RFA is the duration of pain relief it can provide. While individual results vary, many patients experience substantial pain reduction for 6-24 months or longer. This extended relief period can dramatically improve quality of life and reduce dependence on pain medications.
Minimally Invasive Nature
As a minimally invasive pain management technique, RFA involves only small needle punctures rather than surgical incisions. This approach significantly reduces the risk of complications, infection, and scarring while allowing for faster recovery times.
Most patients can return to work and normal activities within a few days, compared to weeks or months of recovery required after traditional surgical procedures.
Reduced Medication Dependence
Successful radiofrequency ablation often allows patients to reduce or eliminate their reliance on pain medications, including opioids. This reduction in medication use can lead to improved cognitive function, better sleep, and fewer medication-related side effects.
Repeatability
When the effects of RFA begin to diminish as nerves regenerate, the procedure can typically be repeated safely and effectively. This repeatability provides patients with a long-term pain management strategy that can be adapted to their changing needs over time.
Potential Risks and Considerations
While radiofrequency ablation is generally considered safe, like any medical procedure, it does carry some potential risks and considerations that patients should understand before treatment.
Common Side Effects
Most side effects of RFA are mild and temporary, including:
- Temporary soreness or bruising at the needle insertion site
- Mild swelling or inflammation
- Temporary numbness in the treated area
- Rarely, temporary increase in pain during the first few days
Rare Complications
Serious complications are uncommon but can include infection, nerve damage, or bleeding. These risks are minimized through proper sterile technique, careful patient selection, and experienced procedural skills.
Factors Affecting Success
The success of radiofrequency ablation depends on several factors, including accurate diagnosis, proper patient selection, precise electrode placement, and the specific pain condition being treated. Not all patients are ideal candidates for RFA, which is why thorough evaluation by qualified specialists is essential.
When to See a Specialist
If you’re experiencing chronic pain that has not responded adequately to conservative treatments such as physical therapy, medications, or injections, it may be time to consider radiofrequency ablation. Ideal candidates for RFA typically have:
- Chronic pain lasting longer than three to six months
- Pain that significantly impacts daily activities and quality of life
- Unsuccessful outcomes with conservative treatments
- Positive response to diagnostic nerve blocks
- Desire to reduce dependence on pain medications
Consulting with a board-certified interventional pain management specialist is crucial for determining whether radiofrequency ablation is appropriate for your specific condition. These specialists have the expertise to perform comprehensive evaluations, interpret diagnostic tests, and develop personalized treatment plans.
The complexity of chronic pain conditions requires specialized knowledge and experience to achieve optimal outcomes. A qualified pain management physician can assess your individual situation, discuss all available treatment options, and help you make informed decisions about your care.
Preparing for Your Consultation
When preparing for a consultation about radiofrequency ablation, gathering relevant information can help ensure a productive appointment. Consider bringing:
- Complete medical records related to your pain condition
- List of current medications and previous treatments
- Recent imaging studies (MRI, CT scans, X-rays)
- Pain diary documenting your symptoms and triggers
- Insurance information and referrals if required
Being prepared to discuss your pain history, treatment goals, and concerns will help your physician develop the most appropriate treatment plan for your situation.
The Future of Chronic Pain Treatment
Radiofrequency ablation continues to evolve as technology advances and research expands our understanding of chronic pain mechanisms. Newer techniques, such as cooled radiofrequency and pulsed radiofrequency, offer additional options for treating various pain conditions.
These innovations, combined with improved patient selection criteria and procedural techniques, continue to enhance the effectiveness and safety of radiofrequency ablation as a chronic pain treatment option.
For patients struggling with chronic pain, radiofrequency ablation represents hope for reclaiming their lives and achieving meaningful pain relief. The procedure’s proven track record, combined with its minimally invasive nature and long-lasting effects, makes it an attractive option for many individuals seeking alternatives to traditional pain management approaches.
If chronic pain is affecting your quality of life and limiting your activities, don’t wait to explore your options. The experienced team at Modal Pain Management, led by Dr. Alex Movshis, MD, offers comprehensive evaluation and advanced interventional pain therapy techniques, including radiofrequency ablation NYC patients can trust. Dr. Movshis is a dual board-certified anesthesiologist and interventional pain management specialist trained at the prestigious Icahn School of Medicine at Mount Sinai. To schedule a consultation and learn more about how radiofrequency ablation might help you find relief from chronic pain, call (646) 290-6660 or visit our contact page today.
Frequently Asked Questions
Radiofrequency ablation typically provides pain relief for 6-24 months or longer, depending on individual factors and the specific condition being treated. The procedure can be safely repeated when pain returns as nerves regenerate.
The RFA procedure itself involves minimal discomfort due to local anesthesia and mild sedation. Some patients may experience temporary soreness at the injection site for a few days after the procedure, but this typically resolves quickly.
Good candidates for RFA typically have chronic pain lasting more than 3-6 months that hasn't responded to conservative treatments, positive response to diagnostic nerve blocks, and desire to reduce medication dependence. A comprehensive evaluation by a pain management specialist determines candidacy.