If you are reading this, the pattern probably feels familiar. The C-section was years ago. The incision healed. Then the burning started — sometimes weeks after the surgery, sometimes after a second pregnancy, sometimes seemingly out of nowhere. It is felt at one specific spot on the lateral edge of the Pfannenstiel scar, and it radiates into the mons pubis, the labia, or the upper inner thigh. Tight waistbands make it worse. Sitting cross-legged makes it worse. Sometimes intimacy makes it worse. You have been told it is “scar tissue,” “adhesions,” “post-surgical pain,” “endometriosis,” “pelvic floor dysfunction,” or — worst — “stress.” Maybe you have had a laparoscopy that found nothing. Maybe you have been on pelvic-floor physical therapy that hasn’t moved the dial.
This post is about what that pain actually is, why it gets misdiagnosed for years, and how a 15-minute diagnostic procedure usually identifies the source and starts treating it.
Why this gets missed
There are three reasons chronic Pfannenstiel-incision nerve pain gets misdiagnosed for years.
First, the differential default for chronic lower-abdominal pain in a woman of reproductive age is gynecologic. The first stop after the primary care visit is a gynecologist. The standard workup — pelvic exam, transvaginal ultrasound, laboratory studies, often a diagnostic laparoscopy — is structured to find endometriosis, adenomyosis, ovarian pathology, fibroids, or pelvic adhesive disease. It is not structured to evaluate abdominal-wall neuropathy. A negative pelvic workup typically yields a diagnosis of “chronic pelvic pain of unclear etiology” or a presumed endometriosis without histologic confirmation. The patient ends up on hormonal suppression and physical therapy. Neither addresses a peripheral nerve generator.
Second, the pain mimics conditions that are far more commonly diagnosed. Endometriosis has a real epidemiologic prevalence of roughly 10% in women of reproductive age. Chronic post-Pfannenstiel nerve entrapment has a meaningful but smaller prevalence — published case series put the rate at 3–7% of patients with persistent scar-region pain after Pfannenstiel surgery. Bayesian reasoning makes endometriosis the leading hypothesis by default. The clinical features that point to nerve entrapment — burning quality, positive Tinel sign, no cyclical fluctuation, no menstrual aggravation — are not part of the routine gynecologic exam.
Third, the right diagnostic test is not part of the gynecologic workflow. An ultrasound-guided TAP-plane block at the lateral edge of the Pfannenstiel scar is performed in pain medicine clinics with image-guided procedural infrastructure. It is not part of an obstetric or gynecologic practice. The patient who needs this test is rarely referred for it. The result is a multi-year diagnostic loop where the right test is never run.
The diagnostic workflow that actually solves this: cutaneous mapping (which dermatomes are affected — ilioinguinal supplies the inguinal crease and base of labia; iliohypogastric supplies a band above the inguinal ligament), Tinel testing along the upper edge of the Pfannenstiel scar, and an ultrasound-guided block at the Tinel-positive level. Three steps, one visit, diagnostic answer in 30 minutes from check-in to walk-out.
The anatomy that matters
The Pfannenstiel incision is a transverse, low, suprapubic incision used for cesarean section, benign hysterectomy, and pelvic reconstructive surgery. It is typically 10–15 cm long, made 2–4 cm above the pubic symphysis, with fascia closed in layers including the rectus sheath. The skin incision is cosmetic; the underlying fascial closure is where the nerves get caught.
The ilioinguinal nerve (L1) and the iliohypogastric nerve (T12–L1) both cross the Pfannenstiel surgical field at the lateral edges of the incision. They run between the internal oblique and transversus abdominis muscles in the transversus abdominis plane (TAP), then pierce the rectus sheath to supply the overlying skin. At the lateral edge of the rectus sheath — typically 5–8 cm lateral to the linea alba — they make a 90° turn from the TAP plane into the subcutaneous tissue. That 90° turn is the anatomic vulnerability. Suture closure of the lateral rectus sheath can entrap the nerve. Scar formation around the suture can compress it. The result is a Tinel-positive point at exactly that 5–8 cm lateral position.
The genitofemoral nerve (L1–L2) is anatomically less commonly involved with Pfannenstiel surgery than with inguinal hernia repair, but it can be irritated by deeper retraction during pelvic dissection — particularly in patients who had concurrent pelvic node dissection or extensive bladder reflection.
In clinical examination, the Tinel-positive point is the single most useful diagnostic clue. You ask the patient to identify the most tender spot on the scar; you palpate it; gentle tapping with a fingertip at that point reproduces the patient’s typical burning radiating pain. A focal point that consistently reproduces the radiating quality of the pain is diagnostic for nerve entrapment until disproved by a block.
How we diagnose
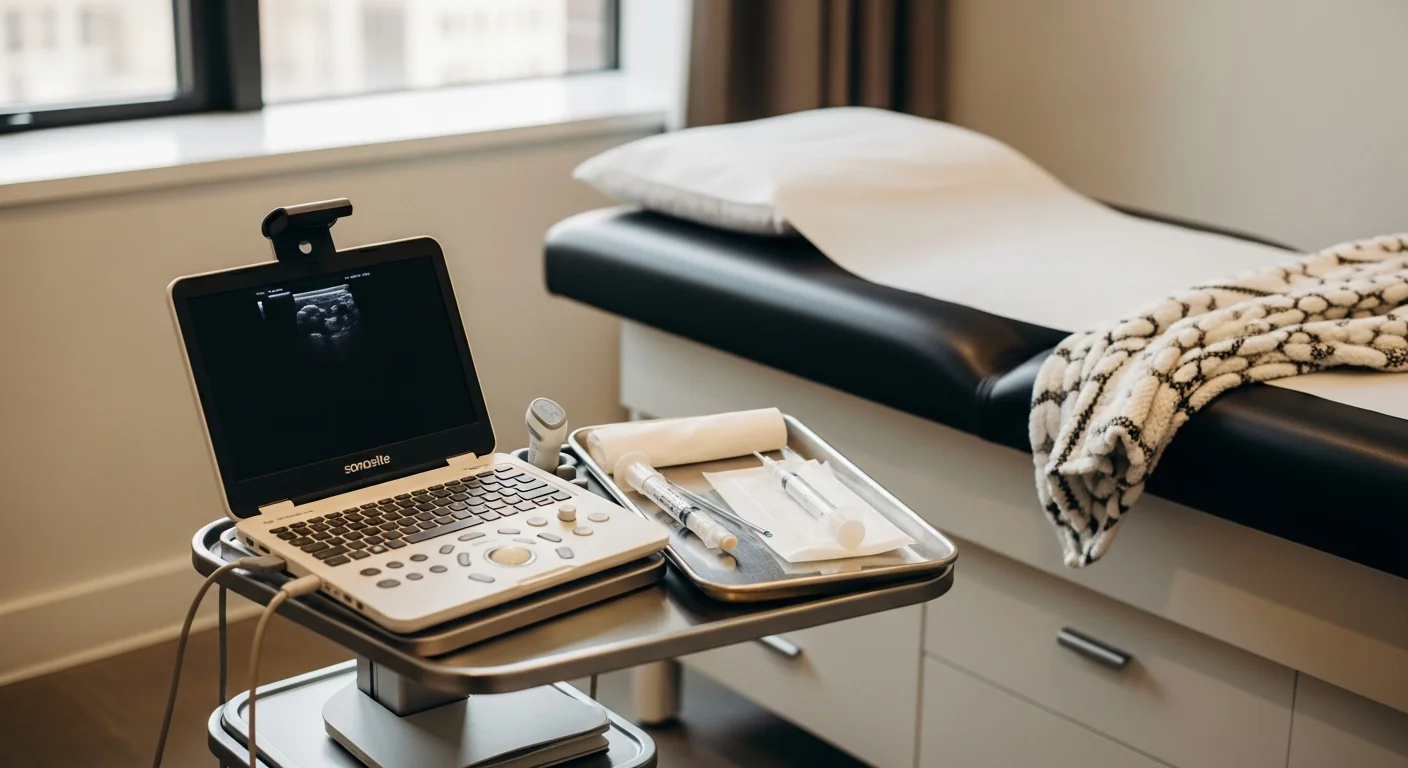
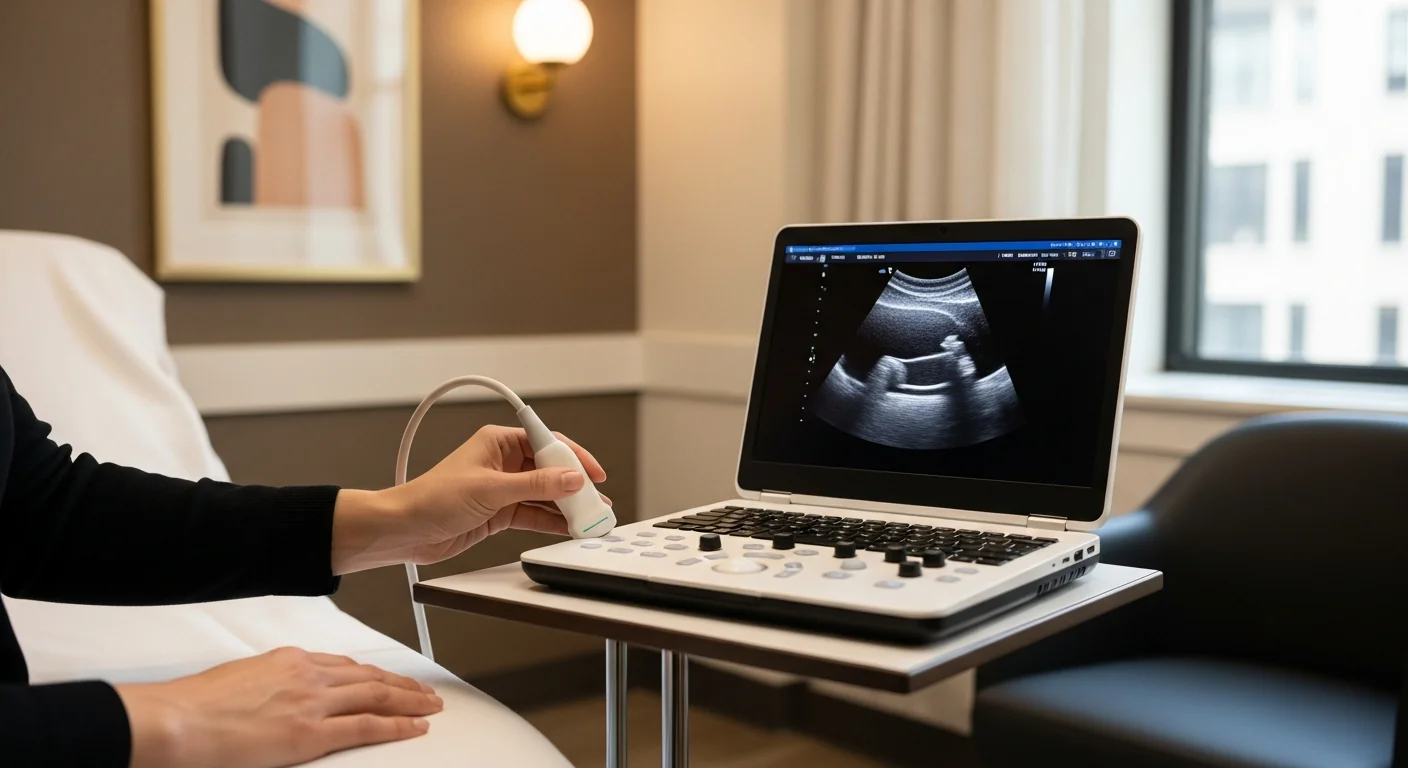
The diagnostic procedure is an ultrasound-guided TAP-plane nerve block at the Tinel-positive level. Performed in our procedure suite at 369 Lexington Avenue. Total visit time from check-in to walk-out: about 30 minutes.
Technique: with the patient supine, the abdominal wall anatomy is identified by ultrasound (external oblique, internal oblique, transversus abdominis, and the lateral edge of the rectus sheath at the Tinel-positive level). A 22-gauge needle is advanced under direct ultrasound visualization into the TAP plane between the internal oblique and transversus abdominis at the Tinel-positive level. After negative aspiration, 4–5 mL of 0.5% bupivacaine plus 20–40 mg of triamcinolone is delivered. Spread is observed in real time — a successful injection produces a hypoechoic plane between the two muscle layers along the lateral incision edge.
The diagnostic effect is immediate. Within 10–15 minutes, the burning pain should abolish or substantially decrease. ≥50% pain abolition compared with the patient’s baseline is a positive block; ≥75% is highly specific. The patient keeps a pain diary every 30 minutes for the next four hours and at intervals over the next several days, which informs the therapeutic duration.
The therapeutic effect with corticosteroid added typically lasts 4–12 weeks. Patients who respond to the diagnostic block and want durable treatment have several options on the ladder:
- Repeat therapeutic blocks every 8–12 weeks during the period of active pain modulation
- Ultrasound-guided hydrodissection (volume injection of saline or 5% dextrose) to mechanically separate the nerve from fascial scar — particularly effective when the nerve is bound by dense scar at the rectus-sheath edge
- Pulsed radiofrequency ablation of the affected nerve for 6–12 months of relief at a time, repeatable as the nerve regenerates
The diagnostic block is the gate that opens this whole ladder. Without it, the workup defaults to the wrong differential.
Treatment ladder and when surgery is the right call
For most patients with confirmed Pfannenstiel-incision nerve entrapment, the treatment ladder ends at therapeutic blocks or pulsed RFA. A meaningful minority — patients with deeply scarred fascial entrapment, large neuromas, or severely refractory disease — escalate to surgical management.
Step 1 — neuropathic-pain medication. Gabapentin or pregabalin, titrated. Tricyclic antidepressant or SNRI for patients who do not tolerate gabapentinoids. Topical 5% lidocaine patch over the Tinel-positive band is highly effective and underused.
Step 2 — ultrasound-guided diagnostic and therapeutic nerve block. The workhorse described above.
Step 3 — ultrasound-guided hydrodissection. Volume injection of saline or 5% dextrose to mechanically free the nerve from the surrounding fascial scar. Often dramatic in benefit and durable for patients with adhesion-bound nerves.
Step 4 — pulsed radiofrequency ablation. For patients with clear positive blocks and diminishing therapeutic duration. Pulsed (neuromodulatory, not destructive) is essential because the territory innervated is in cosmetically and sexually sensitive skin.
Step 5 — peripheral nerve stimulation referral. Percutaneous PNS at the affected nerve for refractory cases. FDA-cleared with published case-series support.
Step 6 — surgical neurectomy by peripheral nerve plastic surgery. When the conservative ladder reaches its ceiling, the durable salvage is operative. The procedure transects the ilioinguinal and iliohypogastric nerves proximal to the scar — typically through a small retroperitoneal approach away from the original incision — and implants the proximal stumps into muscle to prevent recurrent neuroma formation. Performed by a peripheral nerve plastic surgeon (not the original obstetric or gynecologic surgeon), published case series report 70–85% meaningful pain relief at 12 months. Modal Pain coordinates the referral directly and provides the surgical team with the documented diagnostic-block response, the operative report from the index Pfannenstiel surgery, and any imaging that has been performed.
Surgery is not the goal of treatment. The goal is to identify the pain generator and treat it with the least invasive durable intervention. Surgery is what we coordinate for the small subset of patients whose nerve has been chronically entrapped and damaged to the point that block-and-modulate strategies cannot keep up.
For referring physicians
When referring a patient with persistent Pfannenstiel-scar pain >3 months after C-section, hysterectomy, or low-transverse pelvic surgery, send: the operative report from the index surgery, any post-operative imaging (transvaginal ultrasound, MRI of the pelvis), the patient's prior medication trial history, and a note on whether the pain is cyclical (suggests endometriosis component) or non-cyclical with burning quality (suggests neuropathic). We document a Tinel test at the consultation, run an ultrasound-guided diagnostic block at the lateral incision edge, and send notes back to the referring gynecology or obstetrics practice after each visit. For the small fraction of patients whose diagnosis is confirmed but who fail the conservative ladder, we coordinate the peripheral nerve plastic surgery referral and provide the surgical team with the diagnostic documentation they require.
Ready to evaluate your post-Pfannenstiel pain
If your C-section scar pain has persisted more than three months and a gynecologic workup has not produced an answer, the next step is an image-guided diagnostic block. Same-week new-patient consultations are available at 369 Lexington Avenue in Midtown Manhattan.
Verify your insurance covers a post-Pfannenstiel pain workup Book a same-week diagnostic block
Or call (646) 290-6660.
For the broader framework on chronic post-surgical nerve pain, see the post-surgical and iatrogenic nerve pain page.
Frequently Asked Questions
Yes, and this is common enough that we see it frequently. Most chronic C-section scar pain begins within the first 2–8 weeks after surgery, but a meaningful subset of patients develop delayed-onset pain months or even years later — typically triggered by a second pregnancy, a weight change, an unrelated abdominal surgery, or a postural change. The mechanism is the same: an ilioinguinal or iliohypogastric nerve has been chronically irritated by suture or scar at the lateral edge of the Pfannenstiel incision, and a triggering event tips it from asymptomatic into symptomatic.
Quality and pattern. Nerve pain is burning, electric, lancinating, or 'stabbing,' often with allodynia (light touch to the affected skin hurts). Adhesion pain is dull, deep, and dragging — worse with motion, often crampy. Nerve pain has a positive Tinel sign: tapping at a specific point on the lateral incision edge reproduces the radiating pain. Adhesion pain does not have a Tinel sign. The diagnostic block — ultrasound-guided TAP-plane block at the lateral incision edge — abolishes nerve pain in 15 minutes and does not change adhesion pain. The test sorts them out cleanly.
Scar endometriosis is a real entity — but it produces cyclical pain (worse during menses), a palpable tender mass within the scar that enlarges around menstruation, and is confirmed by ultrasound showing a discrete hypoechoic nodule. Most patients who present with chronic Pfannenstiel pain have neuropathic features (burning, allodynia, positive Tinel) without cyclical fluctuation and without a discrete mass on ultrasound. The neuropathic pattern is far more common. Both diagnoses can coexist, and both have specific image-guided treatment options.
Ultrasound-guided injection of 4–5 mL of 0.5% bupivacaine plus 20–40 mg of triamcinolone into the transversus abdominis plane (TAP) at the lateral edge of the rectus sheath, at the Tinel-positive level. The diagnostic effect is immediate — within 10–15 minutes, the burning pain should abolish or substantially decrease. The therapeutic effect with steroid added typically lasts 4–12 weeks. If diagnostic-only is needed (insurance authorization or patient preference), bupivacaine alone gives 4–24 hours of diagnostic relief.
For refractory cases not responding to image-guided blocks, hydrodissection, and pulsed RFA, peripheral nerve neurectomy by a peripheral nerve plastic surgeon is the durable salvage option. Published case series report 70–85% meaningful pain relief at 12 months. The procedure transects the ilioinguinal and iliohypogastric nerves proximal to the scar and implants the stumps into muscle to prevent recurrent neuroma. It is not the first move — most patients respond to interventional treatment without surgery — but it is a real option when needed.
No. Image-guided ilioinguinal and iliohypogastric blocks have no effect on fertility, pregnancy, or labor. Pulsed RFA at the same nerves is also pregnancy-compatible. Surgical neurectomy, when needed, leaves the rest of the abdominal wall and uterus completely undisturbed. The vast majority of patients with Pfannenstiel nerve entrapment have one or more additional pregnancies after treatment without complication.
Most commercial PPO plans cover image-guided peripheral nerve blocks for chronic post-surgical pain, typically with prior authorization. Modal Pain Management verifies your benefits before the first visit. We accept most major commercial PPO plans and do not participate with Medicare or Medicaid. <a href="/verify-insurance/">Check your plan</a> or call (646) 290-6660.