If you have a defined patch of burning, tingling, or hypersensitive skin on the front and outer thigh that you can outline with one finger, that does not cross the knee, that gets worse with tight waistbands or long stretches of standing, and that has been called “sciatica” or “L2-L3 radiculopathy” for months without an MRI finding to back that up — you are reading the right post. The condition is meralgia paresthetica. It is a peripheral nerve entrapment, not a spine problem. A 15-minute ultrasound-guided block at the inguinal ligament both confirms the diagnosis and treats it.
Why this gets missed
Meralgia paresthetica is the most commonly missed entrapment neuropathy in adults. The classic reason is the differential default: any leg pain in a working-age adult gets routed through lumbar spine MRI first, where mild degenerative findings (and almost every adult has some) get blamed for the pain. The patient ends up on a lumbar PT protocol that does nothing for an inguinal-ligament entrapment.
The Cheatham and Pearce reviews document the diagnostic delay. Mondelli’s case-control work links the condition to BMI but the broader population — pregnant women, weightlifters with tight tactical belts, long-distance cyclists, post-anterior-hip-arthroplasty patients, and now GLP-1 weight-loss patients — gets workups aimed at the wrong target. The single most useful question in the differential is: does the pain cross the knee? Meralgia paresthetica never does. Sciatica and L2-L3 radiculopathy can.
The second most useful question: is there any motor weakness? The LFCN is a pure sensory nerve. Quadriceps weakness, hip-flexor weakness, foot drop, ankle dorsiflexion weakness — any of these rules out meralgia paresthetica and points back to the spine.
The anatomy that matters
The lateral femoral cutaneous nerve arises from L2-L3, crosses the iliac fossa, and passes under (or, in 15–25% of the population, through) the inguinal ligament approximately 1 cm medial to the anterior superior iliac spine (ASIS). Distal to the inguinal ligament, the nerve becomes subcutaneous and supplies the skin of the anterolateral thigh from the inguinal crease down to the knee — but not past it.
Three mechanical things tighten the inguinal ligament over the LFCN: weight gain (especially central adiposity), anterior pelvic tilt, and prolonged hip extension. Three mechanical things pull on or trap the nerve directly: tight waistbands at the ASIS level (skinny jeans, tactical belts, weightlifting belts, low-rise tight clothing), pregnancy in the second and third trimesters, and post-surgical scar after anterior approach total hip arthroplasty or iliac crest bone graft harvest.
Rapid weight loss — including GLP-1-mediated weight loss — is the newer mechanical trigger. The mechanism is the inverse of weight gain: the tissue planes around the inguinal ligament shift as fat is lost, the ligament’s geometry over the nerve changes, and the nerve becomes mechanically irritated. It’s a real pattern in our practice. The published literature linking GLP-1 specifically is still emerging.
How we diagnose
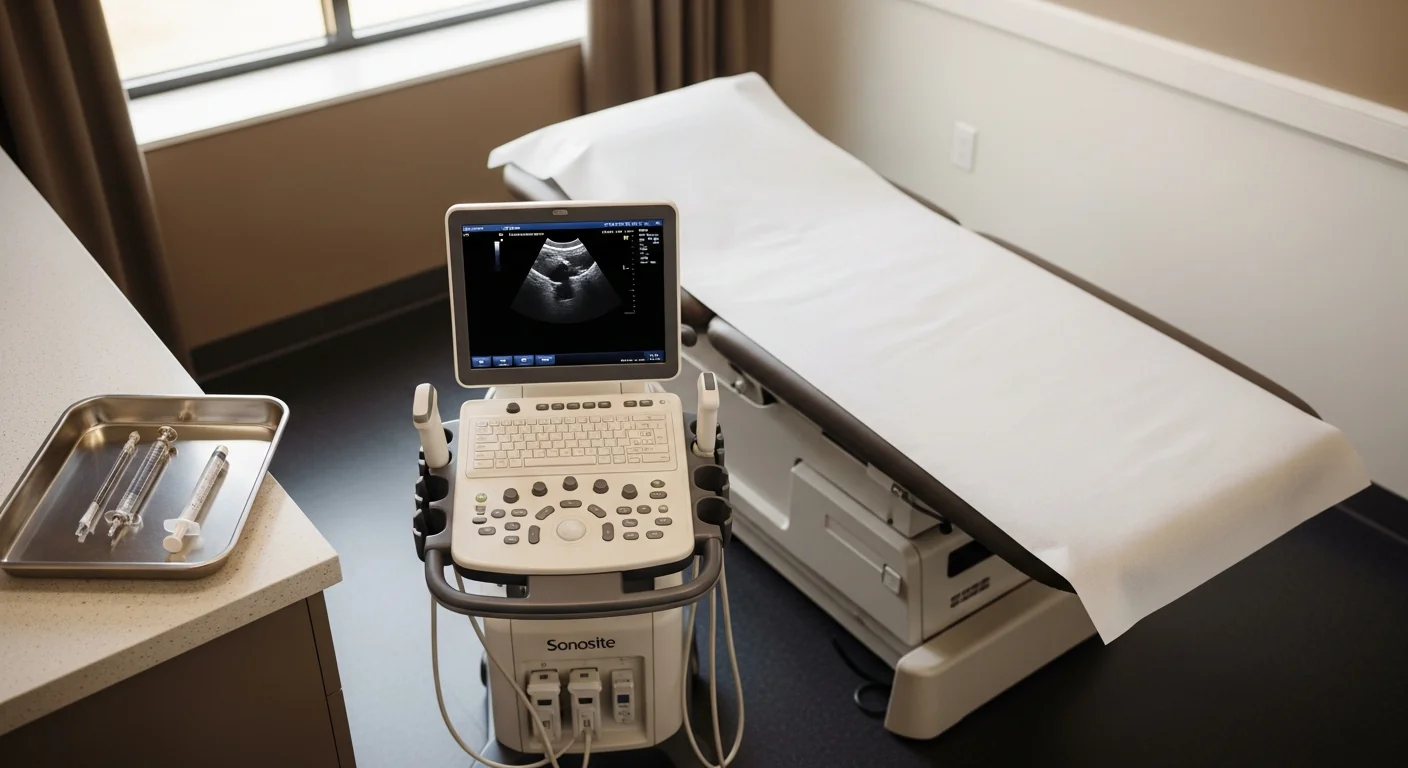
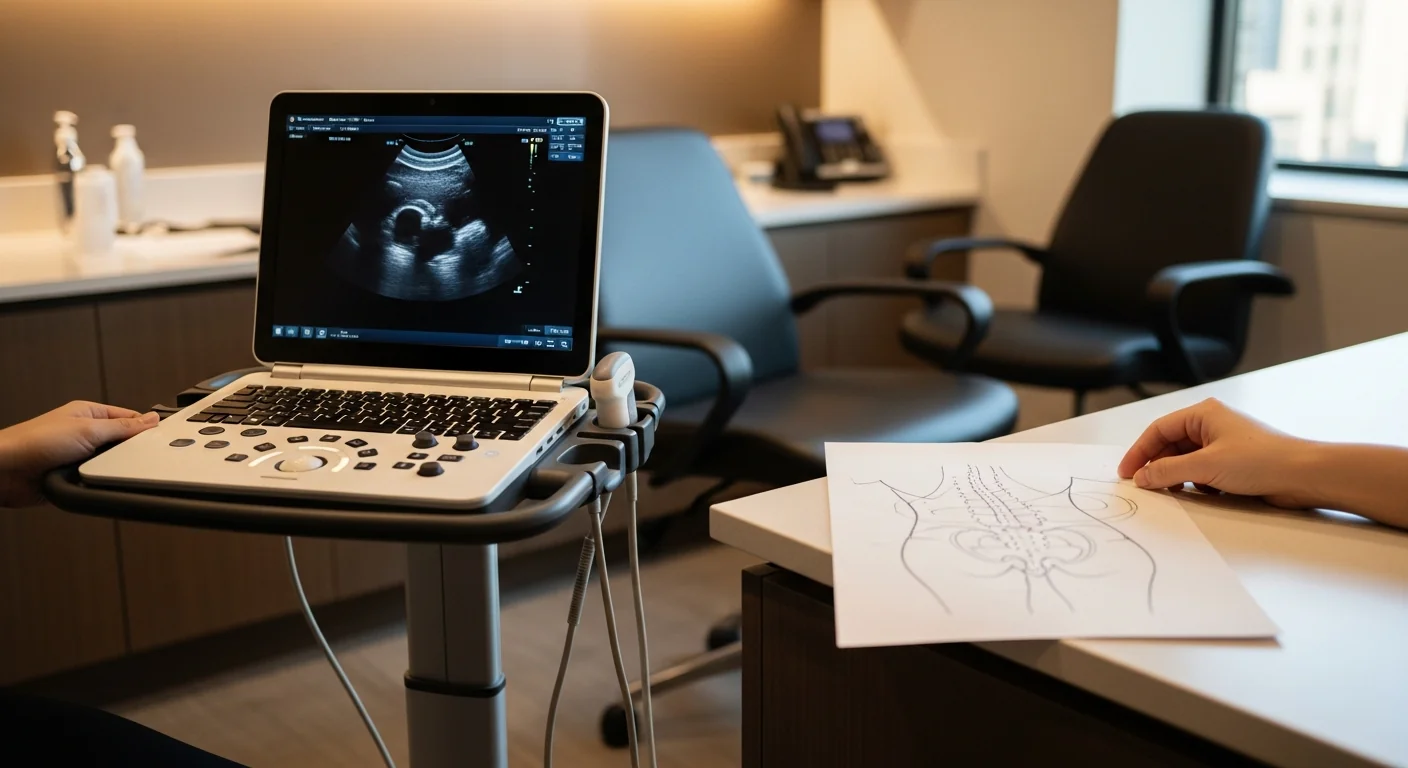
The diagnostic procedure is an ultrasound-guided LFCN block at the inguinal ligament. Total visit time from check-in to walk-out: about 30 minutes.
Technique: with the patient supine, the inguinal anatomy is identified on ultrasound — the ASIS, the inguinal ligament, the sartorius muscle inferior to the ligament, and the LFCN where it passes between them. A 22-gauge needle is advanced under direct ultrasound visualization into the fascial plane immediately deep to the inguinal ligament. After negative aspiration, 3–5 mL of 0.5% bupivacaine plus 20 mg of triamcinolone is delivered, with spread observed in real time.
The diagnostic effect arrives within 10–15 minutes. ≥75% relief of the typical anterolateral thigh burning is the definitive test for meralgia paresthetica. The therapeutic effect with corticosteroid added typically lasts 6–12 weeks. Patients keep a pain diary every 30 minutes for four hours and at intervals over the next several days, which informs the next step.
Treatment ladder and when surgery is the right call
Step 1 — remove the mechanical compressor when one exists. Tight waistbands, tactical belts, low-rise pants. Pregnancy-related cases often resolve postpartum without intervention. Weight-driven cases improve with central weight loss. GLP-1-driven cases are managed without stopping the medication.
Step 2 — neuropathic-pain medication trial plus targeted PT. Gabapentin or pregabalin at standard titration. Topical 5% lidocaine patch over the affected territory is highly effective and underused. Targeted PT focuses on three specific moves rather than generic stretching — iliopsoas extension stretching in a kneeling lunge, hip-flexor balance work, and glute-medius activation to correct anterior pelvic tilt.
Step 3 — ultrasound-guided LFCN block with corticosteroid. The workhorse procedure. Diagnostic in 15 minutes, therapeutic for 6–12 weeks.
Step 4 — hydrodissection of the LFCN. Volume injection of saline or 5% dextrose to mechanically separate the nerve from fibrotic tissue planes — particularly effective in post-surgical and post-traumatic cases.
Step 5 — pulsed radiofrequency ablation of the LFCN. For chronic refractory cases with documented positive blocks. Pulsed (not conventional thermal) RFA is essential because the territory is cosmetically sensitive. 6–12 months of relief per treatment.
Step 6 — surgical decompression. Refractory cases get referred for Dellon-style external neurolysis of the LFCN at the inguinal ligament, performed by peripheral nerve plastic surgery. The procedure releases the ligament’s compressive band on the nerve. Published case series report 70–85% meaningful pain relief at 12 months. Modal Pain coordinates the referral directly and provides the documented diagnostic-block response surgical programs require.
The point of the ladder is to treat the mechanical generator at the lowest invasive level that works. Most patients respond to medication + block + targeted PT. Surgery is for the small fraction that doesn’t.
For referring physicians
When referring a patient with anterolateral thigh burning that does not cross the knee, send: the lumbar spine MRI report (if one was done — most cases do not need it), the medication trial history, any recent weight-change information (including GLP-1 prescription history), and a note on the cutaneous distribution. We document a Tinel sign at the inguinal ligament, perform an ultrasound-guided LFCN block in the room, and send notes back to the referring physician after each visit. For refractory cases meeting criteria, we coordinate peripheral nerve plastic surgery referral directly.
Ready to evaluate your outer thigh pain
If you have burning anterolateral thigh pain that does not cross the knee and no motor weakness, an image-guided LFCN block is the diagnostic answer. Same-week new-patient consultations are available.
Verify your insurance covers a meralgia paresthetica workup Book a same-week diagnostic block
Or call (646) 290-6660.
For the broader framework on peripheral nerve entrapments, see the peripheral nerve entrapment page.
Frequently Asked Questions
No. Meralgia paresthetica is uncomfortable but not dangerous. The lateral femoral cutaneous nerve (LFCN) is a pure sensory nerve — it does not affect muscle strength, walking, or any bodily function. There is no risk of paralysis, no risk of permanent damage if untreated, and no medical emergency. The pain itself can be intense and disabling, but the condition does not progress to something worse. The reason to treat it is quality of life, not safety.
We're seeing a clear pattern in our practice: patients on GLP-1 weight-loss medications (semaglutide, tirzepatide) presenting with new-onset meralgia paresthetica 3–9 months into rapid weight loss. The likely mechanism is mechanical — rapid loss of intra-abdominal and subcutaneous fat changes the geometry of the inguinal ligament's pull over the LFCN. The treatment ladder is identical to non-GLP-1 cases, and the GLP-1 medication itself does not need to be stopped. The base condition (mechanical compression at the inguinal ligament) was always there; weight loss is just one of several mechanical triggers that includes pregnancy, tight clothing, prolonged hip extension, and post-surgical positioning.
The distribution. Meralgia paresthetica is strictly confined to a patch on the front and outer thigh that does NOT cross the knee, with no motor weakness whatsoever. Sciatica radiates down the back of the leg, often past the knee into the calf and foot, and frequently produces motor weakness in the L4, L5, or S1 dermatomes. L2-L3 radiculopathy can produce similar anterolateral thigh pain but typically also affects hip flexors or quadriceps strength, and MRI of the lumbar spine shows the nerve root compression. A diagnostic block of the LFCN at the inguinal ligament — which abolishes meralgia paresthetica pain in 15 minutes — is the single most efficient way to separate the two.
Not generic stretching. Three specific moves that target the inguinal ligament's pull over the LFCN: (1) iliopsoas stretch in a kneeling lunge with the affected hip in extension — 30 seconds × 3, twice daily. (2) hip-flexor strengthening with the cable column at low intensity to balance the iliopsoas-rectus femoris-sartorius complex around the inguinal ligament. (3) glute medius activation (clamshells, side-lying hip abduction) to correct the anterior pelvic tilt that increases tension over the LFCN. Avoid prolonged hip extension activities — long-distance cycling on a road bike with aggressive geometry is a classic trigger. PT focused on these moves rather than generic 'thigh stretching' produces measurably better outcomes.
Ultrasound-guided injection of 3–5 mL of 0.5% bupivacaine plus 20 mg of triamcinolone immediately deep to the inguinal ligament, 1 cm medial and inferior to the anterior superior iliac spine (ASIS). The LFCN is identified directly on ultrasound in most patients; in patients with anatomical variants, the medication is deposited in the fascial plane immediately deep to the ligament. The diagnostic effect is immediate — ≥75% relief of the typical anterolateral thigh burning within 10–15 minutes is the definitive test. With corticosteroid added, the therapeutic effect typically lasts 6–12 weeks.
Surgical decompression is the salvage option for patients who fail the conservative ladder — medication, image-guided block + steroid, hydrodissection, and pulsed RFA. The procedure is a Dellon-style external neurolysis of the LFCN at the inguinal ligament, performed by a peripheral nerve plastic surgeon. The literature reports 70–85% meaningful pain relief at 12-month follow-up in selected patients. Modal Pain coordinates the surgical referral directly and provides the documented diagnostic-block response that surgical programs require.
Most commercial PPO plans cover image-guided LFCN blocks for chronic meralgia paresthetica, typically with prior authorization. Pulsed RFA requires documented positive response to one or more diagnostic blocks before approval. Modal Pain Management verifies your benefits before the first visit. We accept most major commercial PPO plans and do not participate with Medicare or Medicaid. <a href="/verify-insurance/">Check your plan</a> or call (646) 290-6660.