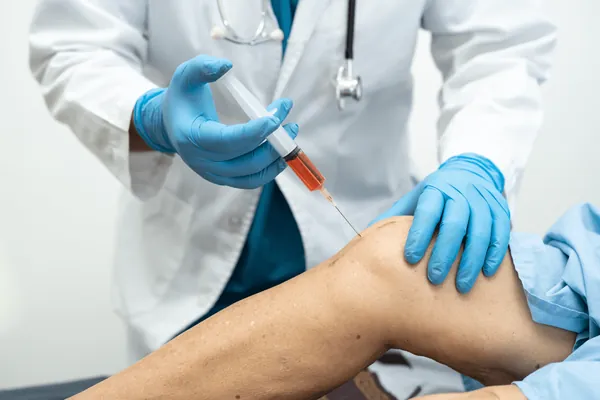
At Modal Pain Management in Midtown Manhattan, Dr. Alex Movshis performs image-guided genicular nerve block and genicular nerve radiofrequency ablation as the most powerful interventional option for chronic knee osteoarthritis pain — a non-surgical alternative to total knee replacement, a bridge for patients delaying or avoiding surgery, and a powerful pain-control option for patients with persistent pain after total knee arthroplasty. The procedure has two phases: a diagnostic genicular nerve block that confirms the genicular nerves as the pain pathway, followed by a therapeutic radiofrequency ablation that produces 6 to 12 months — and frequently longer — of pain relief in 60–80% of correctly selected patients. Located at 369 Lexington Avenue Floor 25 in NYC 10017, we perform both procedures under live ultrasound or fluoroscopic guidance using the published evidence base (Choi 2011 RCT, Davis 2018 multicenter RCT, McCormick COOLIEF studies, and the 2021–2024 meta-analyses) to select the right patient, the right anatomic targets, and the right technology — conventional thermal RFA or cooled-tip COOLIEF RFA — for each individual situation.
What the Genicular Nerves Are — and Why They Matter for Knee Pain
The genicular nerves are small, pure sensory branches that carry pain signals from the knee joint capsule, the synovium, and the periosteum of the distal femur and proximal tibia to the spinal cord and brain. They are not motor nerves — they do not control muscle function, and disrupting them does not affect quadriceps strength, knee flexion, or any aspect of voluntary movement. Anatomic studies (Tran, Franco, and colleagues; Kim and the modern ultrasound mapping series) have consistently identified five primary genicular nerve targets that converge on the knee joint:
The superior medial genicular nerve arises from the femoral nerve and runs along the periosteum of the distal medial femur — the anatomic landmark is the junction of the medial femoral epicondyle and the medial femoral shaft. It carries pain from the medial joint capsule, the medial femoral condyle, and the medial menisco-capsular junction.
The superior lateral genicular nerve arises from the common peroneal nerve and runs along the periosteum of the distal lateral femur — the anatomic landmark is the junction of the lateral femoral epicondyle and the lateral femoral shaft. It carries pain from the lateral joint capsule, the lateral femoral condyle, and the lateral menisco-capsular junction.
The inferior medial genicular nerve arises from the tibial nerve and runs along the periosteum of the proximal medial tibia — the anatomic landmark is the junction of the medial tibial plateau and the medial tibial shaft. It carries pain from the medial menisco-tibial junction, the deep medial collateral ligament, and the pes anserine region.
The inferior lateral genicular nerve arises from the common peroneal nerve and runs along the periosteum of the proximal lateral tibia just below the lateral tibial plateau. It is variably present and is targeted in some protocols (particularly for patients with significant lateral compartment involvement).
The middle (recurrent) genicular nerve arises from the popliteal plexus and innervates the cruciate ligaments and the central portion of the joint. It is targeted in select cases — particularly in patients with persistent post-arthroplasty knee pain.
The standard three-target genicular RFA protocol — superior medial, superior lateral, and inferior medial — is the protocol used in the foundational randomized trials (Choi 2011, Davis 2018) and produces the published 60–80% response rate. The five-target extended protocol — adding the inferior lateral and middle genicular nerves — is used by some clinicians for refractory cases or for post-arthroplasty pain. Modal Pain Management selects the protocol based on the individual clinical picture, the imaging, the response to the diagnostic block, and the published evidence supporting each target.
The clinical importance of the genicular nerve anatomy is this: the pain of knee osteoarthritis is generated by inflamed synovium, exposed subchondral bone, irritated joint capsule, and degenerated menisci, but the pain signal from all of these structures travels through the genicular nerves to reach the brain. By disrupting the genicular nerves with a controlled radiofrequency lesion, the pain signal is interrupted — without altering the joint itself, without surgery, and without damaging any motor function. This is the central insight that makes genicular nerve RFA possible.
How the Procedure Works: Two Phases
The genicular nerve RFA pathway is intentionally structured as two sequential phases — a diagnostic block first, a therapeutic ablation second — to ensure that only patients who have demonstrably responded to silencing of the genicular nerves go on to receive the more durable lesion.
Phase 1 — Diagnostic Genicular Nerve Block
Under live ultrasound or fluoroscopic guidance, Dr. Movshis advances a small-gauge needle to the precise anatomic location of each target genicular nerve (typically the superior medial, superior lateral, and inferior medial branches, performed in sequence). Needle position is confirmed in real time on imaging, and 1–2 mL of local anesthetic — typically 0.5% bupivacaine, sometimes mixed with a small amount of contrast for fluoroscopic confirmation — is slowly injected at each target. The total procedure takes 20–30 minutes and is performed without IV sedation in most cases (intentionally — staying awake is important so the patient can give real-time feedback during the post-block anesthetic window).
The patient is given a structured pain diary and instructed to record their typical knee pain on a 0–10 scale every 30–60 minutes for 4–8 hours after the block, along with notes about specific activities (walking, stair use, prolonged standing, kneeling, getting up from a chair) that normally provoke pain. The diagnostic threshold is 50–80% reduction of typical knee pain during the anesthetic window — a threshold that, in the published literature, predicts a high probability of a successful response to therapeutic RFA.
The block itself does not produce durable relief — by design — and the pain returns to baseline within 24 hours as the local anesthetic wears off. The diagnostic value of the block lies entirely in what happens during the anesthetic window.
Phase 2 — Therapeutic Genicular Nerve Radiofrequency Ablation
If the diagnostic block produces 50–80% relief during the anesthetic window, the patient is scheduled for therapeutic RFA — typically 1–2 weeks after the block, after the pain diary is reviewed at a follow-up visit and the response confirmed. The therapeutic procedure is performed under the same sterile prep and image guidance as the block. A specialized radiofrequency cannula — either a conventional thermal RFA needle (typically 10 cm with a 10 mm active tip) or a cooled-tip COOLIEF cannula (with internal saline cooling that produces a larger, more spherical lesion) — is advanced to each anatomic target. Sensory stimulation testing (50 Hz, low-amplitude) is used to confirm the cannula is positioned at the genicular nerve (the patient reports a tingling sensation in the knee at low voltage). Motor stimulation testing (2 Hz, higher amplitude) is used to confirm there is no muscle twitch — a critical safety check that confirms the cannula is not adjacent to a motor nerve.
Once the position is confirmed, the lesion is created. Conventional RFA delivers radiofrequency energy at 80°C for 90 seconds per target. Cooled-tip COOLIEF RFA delivers energy at 60°C for 150 seconds per target (the lower temperature is possible because of the active internal cooling, which prevents tissue charring at the needle-tissue interface and allows more total energy delivery into a larger volume of tissue). A small amount of local anesthetic is injected at each target after the lesion to manage immediate post-procedure soreness. The total therapeutic procedure takes 45–60 minutes. Light IV sedation may be used in patients who request it, but most patients tolerate the procedure with local anesthesia alone.
The lesion produces an immediate disruption of pain signaling at the targeted nerves. Most patients report meaningful pain reduction within 1–2 weeks, with the full effect typically apparent at 4–6 weeks as post-procedure inflammation resolves. The lesion is not permanent — the genicular nerves regenerate over 9–18 months, at which point pain often begins to return and the procedure can be safely repeated with similar efficacy.
The Evidence Base: Why Genicular RFA Is Standard of Care for Moderate-to-Advanced Knee OA
The evidence base supporting image-guided genicular nerve radiofrequency ablation for chronic knee osteoarthritis is among the strongest in interventional pain medicine. Three landmark studies and a series of supporting trials and meta-analyses establish the role of the procedure.
The Choi 2011 randomized controlled trial (published in the journal Pain) was the foundational sham-controlled study. Thirty-eight patients with moderate-to-advanced knee OA underwent diagnostic genicular nerve block; those with 50%+ relief were randomized to either fluoroscopically-guided conventional thermal RFA or sham (needle placement without RFA energy). At 12 weeks, 59% of the RFA group achieved >50% pain reduction compared with 14% of the sham group — a clinically and statistically meaningful difference. The trial established that the clinical benefit of genicular RFA is real, not a placebo effect, and is mediated by the radiofrequency lesion itself.
The Davis 2018 multicenter randomized controlled trial (published in Regional Anesthesia and Pain Medicine) was the larger, head-to-head comparison against the standard-of-care alternative. One hundred fifty-one patients with chronic knee OA pain were randomized to either cooled-tip COOLIEF genicular RFA or intra-articular corticosteroid injection (the most common conservative interventional treatment). At 6 months, 74% of the cooled-RFA group achieved 50%+ pain reduction versus 16% of the corticosteroid group — a five-fold absolute difference. The benefit persisted at 12 and 24 months in long-term follow-up, with patients in the RFA arm showing better function, lower pain scores, and lower opioid use.
The McCormick COOLIEF studies (2017, 2018, and 2019 publications by Tim McCormick, William Maus, and the Stanford group) extended the evidence by characterizing durability, repeatability, and the post-arthroplasty patient population. The studies demonstrated that cooled-tip RFA produces 12+ month durability in the majority of responders, that the procedure can be safely repeated when nerves regenerate, and that patients with persistent pain after total knee replacement frequently respond to the same protocol.
The 2021–2024 meta-analyses (Hong, Sari, Xiao, and colleagues) pool the randomized and prospective cohort evidence and confirm a 60–80% response rate at 6 months in correctly selected patients, with cooled-tip RFA producing larger and more durable lesions than conventional thermal RFA in head-to-head comparisons.
Consensus guidelines from the American Society of Pain and Neuroscience, the International Pain Spine Society, and the major insurance carriers in 2025–2026 recognize image-guided genicular nerve RFA as an evidence-based interventional option for chronic knee osteoarthritis pain that has not responded to conservative measures and intra-articular injection.
Who Is a Good Candidate — and Who Isn’t
Image-guided genicular nerve block and RFA is the right procedure for several specific clinical scenarios, and the wrong procedure for others. The consultation visit at Modal Pain Management produces a clear yes/no/with-modifications answer for each patient.
The strongest candidates for genicular nerve RFA are: patients with moderate-to-advanced knee osteoarthritis (Kellgren-Lawrence grade 2–4) whose pain has plateaued on the standard non-surgical ladder of weight management, physical therapy, and at least one round of image-guided intra-articular corticosteroid or hyaluronic acid (viscosupplementation) injection; patients in their 50s and early 60s who want to delay total knee replacement for years rather than undergo it now (because knee implants have a finite lifespan and revision surgery is harder than the index procedure); patients who carry high surgical risk from cardiac disease, advanced age, anticoagulation, or other medical comorbidities and for whom TKA is not a safe option; and patients with persistent pain after total knee arthroplasty in whom infection, instability, malalignment, and component issues have been excluded (an emerging high-value indication where genicular RFA can deliver meaningful pain control without surgical revision).
The procedure also has a role for patients with chronic recurrent knee bursitis in whom the joint capsule itself contributes substantially to the pain pattern, and for patients with post-traumatic chronic knee pain after a remote injury that has not responded to conservative care.
The procedure is not the right first-line treatment for: early mild knee OA (where intra-articular corticosteroid, hyaluronic acid, or PRP is more appropriate); knee pain that is primarily mechanical (true locking, true giving way, large meniscal tears in younger patients, ligament instability — these are surgical or sports-medicine problems); acute knee injuries; pain that is clearly referred from the hip or lumbar spine; suspected septic arthritis (a surgical emergency); active gout or pseudogout (treat the crystal arthropathy first); and patients on uncontrolled anticoagulation or with active local infection.
The diagnostic block itself helps sort out the right answer for borderline candidates — if a patient does not respond meaningfully to the diagnostic block, the genicular nerves are not the dominant pain pathway and the workup redirects to other interventions.
Comparison: Genicular RFA vs. Other Knee OA Treatments
Patients evaluating their options for chronic knee osteoarthritis frequently want a side-by-side comparison of where genicular nerve block and RFA fit on the broader treatment ladder.
Compared to image-guided intra-articular corticosteroid injection: corticosteroid produces faster onset (3–7 days) but shorter duration (6–12 weeks); RFA produces slower onset (1–6 weeks) but much longer duration (6–12+ months). Steroid is a better choice for acute flares and fast functional improvement; RFA is a better choice for chronic, ongoing pain control.
Compared to image-guided hyaluronic acid (viscosupplementation, “gel injection”): HA produces 4–6 months of relief and acts on the joint itself (lubrication, synovial environment); RFA produces 6–12+ months of relief and acts on the pain pathway (without altering the joint). The two are complementary — many patients benefit from both, sequentially or in combination.
Compared to image-guided platelet-rich plasma (PRP): PRP has the strongest emerging evidence for medium-term biologic support of mild-to-moderate knee OA and may slow disease progression; genicular RFA is the more powerful interventional pain-control option for moderate-to-advanced disease where the joint is already substantially worn. PRP and RFA target different stages of the disease.
Compared to total knee arthroplasty (TKA): TKA is a definitive surgical procedure that replaces the worn joint surfaces with a metal-and-polyethylene implant — a powerful intervention that produces durable pain relief and functional improvement for the right patient, with a 1–2% major complication rate and a 15–25 year implant lifespan. Genicular RFA is a minimally invasive non-surgical procedure that does not alter the joint and produces 6–12+ months of pain relief per cycle. TKA is the right answer for severe, end-stage disease in the right surgical candidate; RFA is the right answer for patients who want to delay TKA, who are not surgical candidates, or who have persistent pain after TKA.
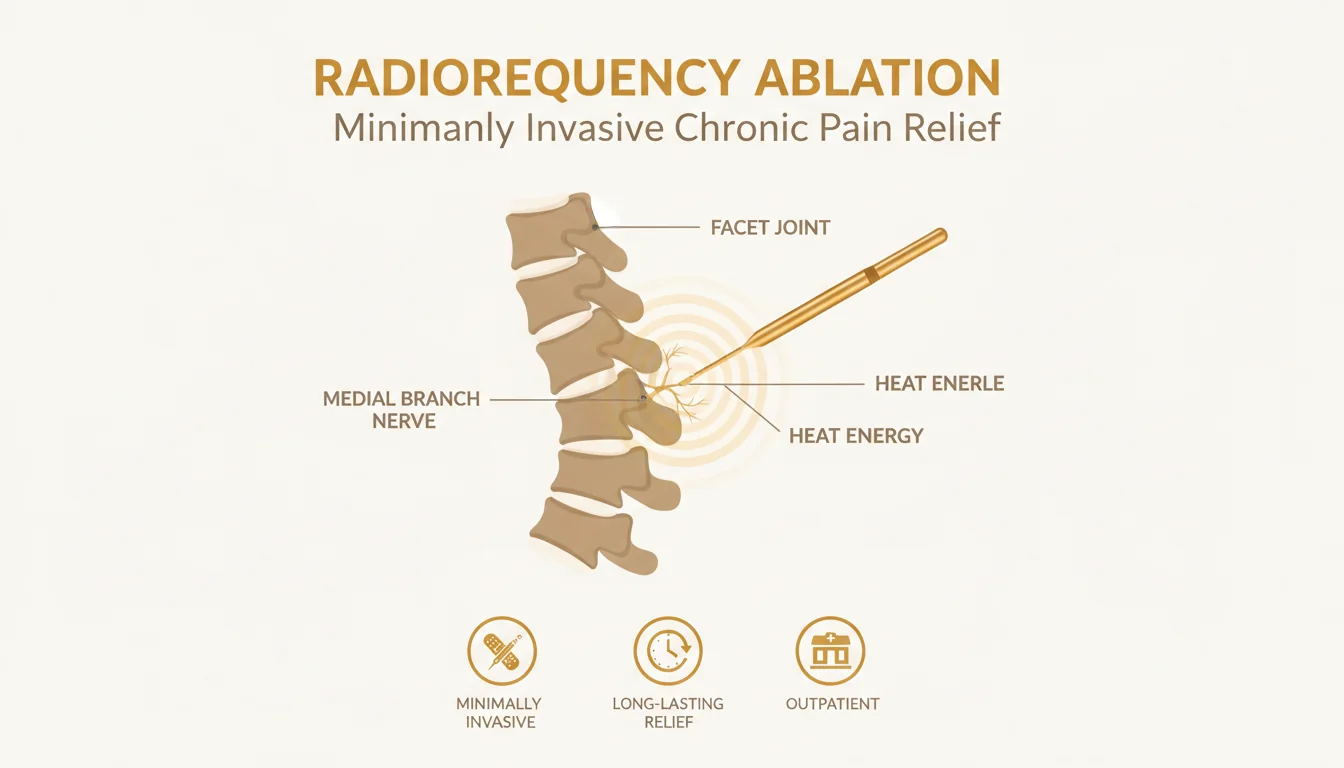
Compared to spinal radiofrequency ablation (the more familiar procedure for back and neck pain): the principles are the same (image-guided thermal lesion of a sensory nerve carrying pain), but the anatomic targets and the indications are different. Spinal RFA targets the medial branch nerves of the facet joints in the cervical, thoracic, or lumbar spine. Genicular RFA targets the genicular nerves of the knee. Both are part of Modal Pain Management’s interventional pain toolkit, and many patients with chronic pain have a combination of spinal and joint pain generators that benefit from coordinated treatment.
Compared to chronic oral pain medication: long-term NSAIDs carry meaningful gastrointestinal, cardiovascular, and renal risks; long-term opioids carry tolerance, dependence, cognitive, and overdose risks. A single cycle of genicular RFA frequently allows patients to substantially reduce or eliminate chronic oral pain medication for the duration of the relief window — a major benefit beyond the pain reduction itself.
What to Expect: The Patient Pathway
The full pathway from initial consultation to therapeutic genicular nerve RFA at Modal Pain Management typically runs 4 to 6 weeks for a new patient. The structured stages are:
Initial consultation visit (45 minutes). Dr. Movshis reviews your knee history, prior imaging (bring weight-bearing knee X-ray, MRI, or CT on CD or via portal), prior treatments and responses, and overall medical context. A structured physical examination of the knee, the contralateral knee, the hip, and the lumbar spine sorts out the dominant pain generator and rules out referred pain. Bedside ultrasound is used to evaluate the joint in real time — assessing the effusion, the suprapatellar bursa, screening for a Baker’s cyst, and grading any synovitis. The diagnostic plan, the indications for genicular nerve block and RFA, the expected response rates, the alternatives, and the cost and insurance picture are discussed in plain language. Most patients leave the consultation with a clear written plan.
Insurance authorization (5–10 business days). Modal Pain’s team submits the prior authorization request to your insurer with the documentation of conservative care, the clinical examination findings, and the imaging. Most commercial PPO plans approve genicular nerve block and RFA when the documentation supports the indication.
Diagnostic genicular nerve block (20–30 minute procedure). Performed in our Midtown NYC office under live ultrasound or fluoroscopic guidance, with no IV sedation in most cases. You drive home after a 15–20 minute observation period. You record your pain in a structured pain diary every 30–60 minutes for 4–8 hours after the block.
Pain diary review (15-minute follow-up, 1–2 weeks after the block). The diary is reviewed and the response objectively measured. If 50–80% reduction of typical knee pain occurred during the anesthetic window, you proceed to therapeutic RFA. If not, the workup redirects.
Therapeutic genicular nerve RFA (45–60 minute procedure). Performed in the same Midtown NYC office under live image guidance. Conventional thermal or cooled-tip COOLIEF technology is selected based on the clinical picture and insurance coverage. Sensory and motor stimulation confirm correct positioning before the lesion is created. You are observed for 30 minutes after the procedure and discharged with post-procedure instructions, typically taking the rest of the day off and resuming normal activities the following day.
Recovery (1–6 weeks). Mild post-procedure soreness for 3–7 days, managed with over-the-counter analgesics. Pain reduction typically begins within 1–2 weeks and reaches its full effect at 4–6 weeks as post-procedure inflammation resolves. Most patients can transition to a maintenance physical therapy program during this window — the pain reduction enables more productive PT.
Long-term follow-up. A follow-up visit at 3 months objectively measures the response, sets expectations for the duration of relief, and discusses any further management. When the genicular nerves regenerate over 9–18 months and pain begins to return, the RFA can be safely repeated with similar efficacy.
Recovery, Activity, and Return to Function
Recovery from genicular nerve block is essentially immediate — patients drive home, may have mild soreness at the procedure sites for 24–48 hours, and resume normal activities the same day.
Recovery from therapeutic genicular nerve RFA is more substantive but still rapid by interventional standards. Post-procedure soreness at the three or four target sites is common for 3–7 days and is managed with acetaminophen and ice. A small number of patients experience a transient post-RFA dysesthesia (pins-and-needles or tingling sensations in the knee) that resolves within 2–4 weeks — this is a benign and self-limited finding.
Activity restrictions are minimal. Most patients take the day of the procedure off, resume desk-based work the following day, and resume light walking the same evening. High-impact loading (running, jumping sports, heavy resistance training) is reasonable to defer for 1–2 weeks while post-procedure inflammation resolves. Driving is permitted as soon as the patient is comfortable — typically the same day for the diagnostic block and within 1–2 days for the therapeutic RFA.
Many patients use the post-RFA pain reduction as an opportunity to engage more productively in structured physical therapy — particularly quadriceps and hip-abductor strengthening, which is the single best evidence-based exercise intervention for knee OA and which is often hard to do consistently when pain is severe. Modal Pain coordinates referrals to physical therapists experienced with the knee-preservation pathway.
Insurance, Authorization, and Practical Logistics
Most commercial PPO insurance plans cover image-guided genicular nerve block and genicular nerve radiofrequency ablation when ordered as part of a structured workup for chronic knee osteoarthritis pain. Coverage typically requires prior authorization that documents you have completed conservative care (weight management, physical therapy, oral anti-inflammatories, and frequently at least one intra-articular knee injection), that your weight-bearing knee X-ray demonstrates degenerative change, and that your clinical picture is consistent with knee joint pain. Modal Pain Management handles the prior authorization process on your behalf — the typical timeline is 5–10 business days from your initial consultation to authorization, and we usually schedule the diagnostic block within the following week.
We accept most major commercial PPO plans (United Healthcare, Aetna, Cigna, BlueCross BlueShield, Oxford, Empire BCBS) and do not accept Medicare or Medicaid. Out-of-pocket cost depends on your individual deductible and coinsurance — we verify your benefits and provide a written estimate before your first procedure so there are no surprises. The cost of the diagnostic block and the therapeutic RFA are billed separately because they are separate procedures performed on different days. Visit our insurance verification page to check your plan, or call (646) 290-6660 for a benefits check.
For patients without insurance coverage or for whom out-of-network self-pay is the right option, transparent self-pay pricing is provided at the consultation visit.
Why Patients Choose Modal Pain Management for Genicular Nerve Block and RFA
Dr. Alex Movshis is board-certified in Anesthesiology with subspecialty fellowship training in Interventional Pain Medicine, and performs image-guided genicular nerve block and radiofrequency ablation under live ultrasound or fluoroscopic guidance — the standard of care endorsed by the American Society of Pain and Neuroscience. Modal Pain Management offers both conventional thermal RFA and cooled-tip COOLIEF RFA, selected based on the individual clinical picture, the published evidence, and the patient’s insurance coverage. We perform the procedures using the standard three-target protocol (superior medial, superior lateral, inferior medial) for the majority of patients and the extended five-target protocol (adding inferior lateral and middle genicular nerves) for refractory cases or post-arthroplasty pain.
The Modal Pain knee-preservation pathway is structured around this central insight: many patients with moderate-to-advanced knee osteoarthritis — including patients who have been told they need a total knee replacement — are excellent candidates for image-guided genicular nerve RFA and can extend the useful life of their native knee by years, with a procedure that has a dramatically more favorable risk profile than surgery and that can be repeated when the nerves regenerate. For patients who are not surgical candidates due to medical comorbidities, and for patients with persistent pain after a technically successful total knee arthroplasty, genicular RFA is frequently the most powerful pain-control option available.
Our Midtown NYC office at 369 Lexington Avenue Floor 25 is one block from Grand Central Terminal, making it accessible from anywhere in the New York metro area. Same-week consultation appointments for new patients are typically available, and we coordinate the full pathway — consultation, prior authorization, diagnostic block, pain diary review, and therapeutic RFA — as a single integrated workflow rather than a series of disconnected appointments.
If you have chronic knee pain, have completed a course of conservative care, want to delay or avoid total knee replacement, are not a surgical candidate due to medical comorbidities, or have persistent pain after a knee replacement and have been told there is nothing more to do — image-guided genicular nerve block and radiofrequency ablation may be the right next step. Learn more about the underlying condition we most frequently treat with this procedure on our knee osteoarthritis page, or book a consultation to discuss whether you are a candidate.