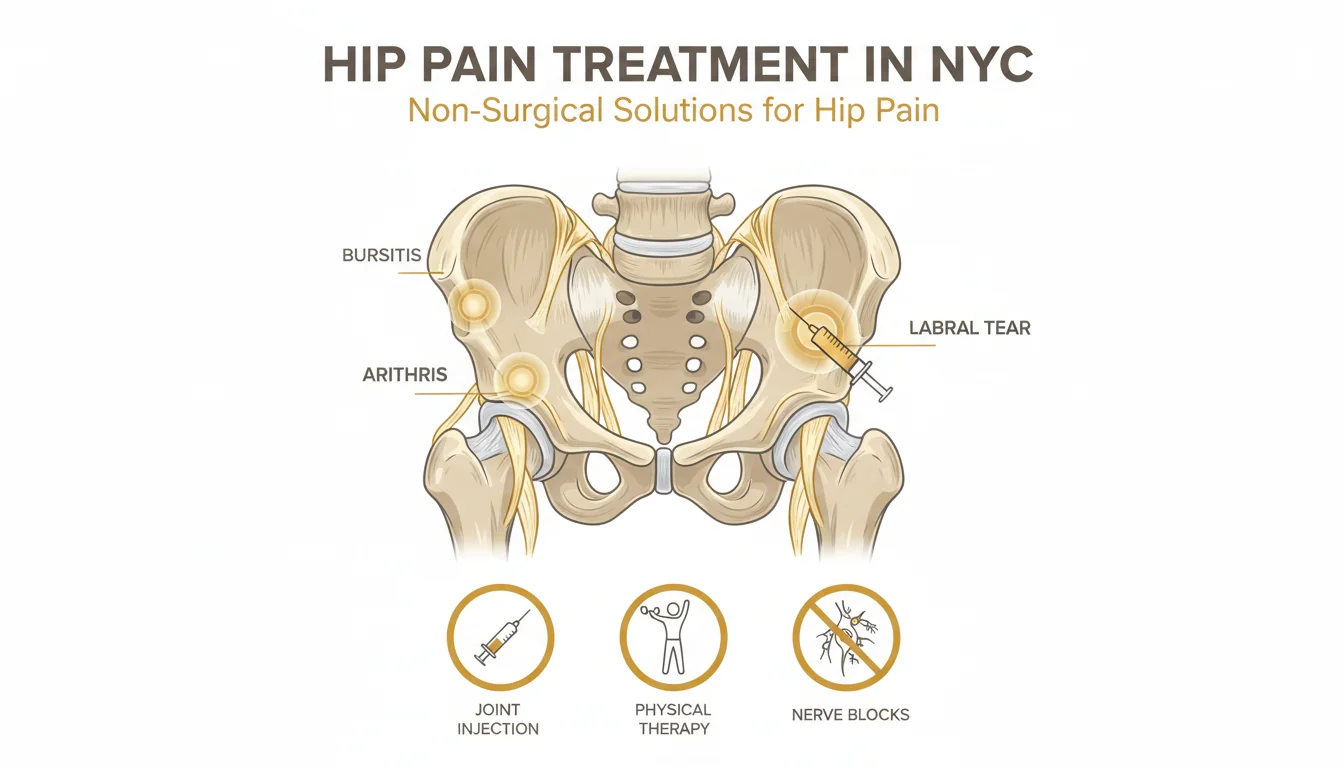
At Modal Pain Management in Midtown Manhattan, Dr. Alex Movshis performs image-guided hip joint injections as the diagnostic gold standard and first-line therapeutic option for hip osteoarthritis, femoroacetabular impingement, acetabular labral tears, and inflammatory hip arthritis. Hip joint pain is one of the most commonly confused musculoskeletal presentations — lumbar radiculopathy, sacroiliac joint dysfunction, trochanteric bursitis, and iliopsoas pathology all produce overlapping pain patterns, and studies have consistently shown that 10–20% of patients presenting with “hip pain” have a non-hip source, while a similar proportion of patients with “low back pain” have hip pathology as the dominant driver. Image-guided injection — performed under live fluoroscopic or ultrasound guidance, with contrast confirmation of intra-articular placement — is the only reliable way to both confirm the hip joint as the pain source and deliver therapeutic medication directly into the intra-articular space. Located at 369 Lexington Avenue Floor 25 in NYC 10017, we perform hip injections using the technique and evidence base endorsed by the Osteoarthritis Research Society International (OARSI) 2019 guidelines, the American Academy of Orthopaedic Surgeons (AAOS), and the Spine Intervention Society (SIS).
The Hip Joint and Why It Hurts
The hip joint is a large ball-and-socket synovial joint formed by the femoral head (the ball, the spherical upper end of the thigh bone) and the acetabulum (the socket, the cup-shaped cavity in the pelvis). The articular surfaces are covered with hyaline cartilage; the joint is lined with a synovial membrane that produces joint fluid; and the joint edge is rimmed by the acetabular labrum, a fibrocartilaginous ring that deepens the socket, increases contact area, and contributes to the joint’s stability and suction-seal mechanics. The joint capsule is dense and heavily innervated, and the surrounding muscles — the gluteal group, the iliopsoas, the adductors, and the deep hip rotators — produce the powerful movements of the hip.
Hip joint pain arises from several overlapping pathologies:
Hip osteoarthritis is the most common indication for image-guided hip injection. Progressive loss of articular cartilage exposes subchondral bone, triggers synovial inflammation, and produces the characteristic pattern of groin pain, anterior thigh pain, and reduced hip internal rotation that defines symptomatic hip OA. Radiographic hip OA affects approximately 15–20% of adults over 45 in the United States; symptomatic hip OA requiring intervention is less common but still clinically significant.
Femoroacetabular impingement (FAI) — an abnormal contact between the femoral head-neck junction and the acetabular rim during hip motion, produced by a cam-type deformity on the femur, a pincer-type overhang on the acetabulum, or both — is an increasingly recognized cause of hip pain in younger, active adults and a known precursor to accelerated hip OA. FAI produces pain with deep flexion and internal rotation (the FADIR-positive pattern) and often damages the acetabular labrum over time.
Acetabular labral tears — tears of the fibrocartilaginous ring at the socket edge — produce catching or clicking sensations, groin pain with pivoting, and pain with deep hip flexion. Labral tears are frequently associated with FAI. Image-guided intra-articular injection is an important diagnostic tool when the labral tear’s clinical relevance is uncertain (the pain-relief response to a diagnostic block confirms the joint itself as the symptom driver, as opposed to extra-articular or referred causes). For more detail on the underlying condition, see our hip labral tear page.
Inflammatory arthritis — rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis-related hip involvement — produces true synovitis of the hip and often responds well to intra-articular corticosteroid as a local adjunct to systemic disease-modifying therapy.
Post-traumatic hip pain — chronic pain after a hip fracture, hip dislocation, or acetabular injury — is a less common but clinically important indication, particularly for patients who have completed orthopedic recovery and have residual mechanical hip pain.
Clinical Evaluation Before Injection
At the consultation visit, Dr. Movshis performs a structured clinical evaluation designed to confirm that the hip joint is the dominant pain source and to characterize the underlying pathology. The evaluation includes:
A pain history that specifically probes for the C-sign (patients cupping the lateral hip with a C-shaped hand, pointing to both groin and lateral pain), pain with weight-bearing, pain with stairs and getting in and out of a car, pain with pivoting, and the functional impact on sleep, work, and daily activity.
A structured physical examination: range of motion testing for the hip (internal rotation is reduced early in hip OA — a specific finding), the FABER test (hip flexion, abduction, external rotation in a figure-four position), the FADIR test (flexion, adduction, internal rotation — positive in FAI and labral pathology), Stinchfield resisted hip flexion (positive in intra-articular pathology), single-leg stance and Trendelenburg test for gluteal function, and a lumbar spine and sacroiliac joint screen to rule out referred pain.
A structured review of imaging: weight-bearing anteroposterior pelvis radiograph and a lateral hip view are the minimum required imaging for any patient being considered for hip injection. MRI is indicated when labral pathology, avascular necrosis, or stress fracture is suspected. CT can be useful for surgical planning in FAI but is less commonly needed for injection decisions.
When the clinical picture supports the hip joint as the dominant pain source, and when conservative measures (physical therapy focused on hip abductor strengthening, oral anti-inflammatories, activity modification) have been attempted without adequate relief, image-guided hip injection is the appropriate next step.
How the Procedure Works
The image-guided hip joint injection is performed in our in-office procedure suite under sterile conditions. The patient is positioned supine (face up) on the procedure table with the affected leg slightly internally rotated — a position that opens the anterior hip capsule and facilitates needle access.
Under live fluoroscopic guidance, a small-gauge spinal needle (typically 22 gauge, 3.5 inches) is advanced through an anterior or anterolateral approach to the femoral head–neck junction, where the anterior capsule attaches. Fluoroscopic confirmation of the bony landmark is performed, 0.5–1 mL of iodinated contrast is injected, and the characteristic intra-articular arthrogram — contrast outlining the femoral head-neck junction and the acetabular recesses — confirms correct placement.
Under ultrasound guidance, the needle is visualized in real time as it advances through the skin and soft tissue to the anterior hip capsule, and intra-articular placement is confirmed by direct visualization of the needle tip within the capsule and observation of the injectate distributing along the femoral neck. Ultrasound-guided hip injection accuracy in experienced hands is well-documented (Deshmukh 2011, Lambert 2007 — 90%+ accuracy).
Once intra-articular placement is confirmed, the therapeutic injectate is slowly delivered. The volume and composition depend on the specific indication:
For corticosteroid injection: typically 1–2 mL of 0.5% bupivacaine (long-acting local anesthetic) mixed with 40–80 mg of triamcinolone or an equivalent long-acting corticosteroid. The local anesthetic provides the diagnostic window (4–24 hours); the corticosteroid provides the 6–12 week therapeutic effect.
For hyaluronic acid viscosupplementation: 2 mL of a cross-linked hyaluronate preparation, delivered either as a single injection or as a series of 3 weekly injections depending on the specific product. Hyaluronic acid is a longer-acting intra-articular option (3–6 months of typical relief) with a different pharmacologic profile than steroid.
For platelet-rich plasma (PRP): the patient’s own blood is drawn at the beginning of the visit, processed in a centrifuge to concentrate platelets 3–8 fold, and the resulting PRP is injected intra-articularly. PRP for hip OA has emerging evidence and is generally self-pay. See our full PRP therapy page.
The total procedure time is 15–25 minutes from skin prep to completion. After the injection, the patient is observed for 15–20 minutes in the recovery area, given a structured pain diary, and discharged with post-procedure instructions.
The Evidence Base
The evidence supporting image-guided corticosteroid hip injection for symptomatic hip osteoarthritis is well-established, though modest in effect size when compared across randomized controlled trials. The 2019 OARSI guidelines provide a conditional recommendation in favor of intra-articular corticosteroid for symptomatic hip OA based on moderate-quality evidence for short-term pain reduction. Multiple randomized trials (Lambert 2007, Atchia 2011, Plant 2014 and others) have demonstrated clinically meaningful pain reduction at 8–12 weeks in correctly selected patients versus placebo or oral analgesic comparators, with 60–70% of patients achieving a meaningful response at 12 weeks.
The evidence for hyaluronic acid viscosupplementation of the hip is weaker than the analogous evidence for the knee and more inconsistent across studies. Several meta-analyses — including the 2018 Saunders review and the 2019 Cochrane review — concluded that the evidence for hip HA is limited and that the effect size is small, though a subset of patients do seem to benefit. Hip HA is reasonable to trial in patients who have responded to corticosteroid but whose relief has shortened, or who prefer to avoid repeated corticosteroid exposure for the reasons discussed in the risk section below.
The evidence for platelet-rich plasma (PRP) for hip OA is still emerging. The 2020–2023 randomized trial base is mixed, with some studies showing benefit comparable to corticosteroid at 6 months and others showing no difference. PRP evidence is substantially stronger for lateral epicondylitis and patellar tendinopathy than for hip OA — see the PRP therapy page for a full evidence discussion.
The evidence for accuracy of image-guided versus blind hip injection is settled. Historical estimates of blind hip injection accuracy range from 50–70%; image-guided accuracy (fluoroscopy or ultrasound in skilled hands) exceeds 90%. Image guidance is considered the standard of care for any diagnostic or therapeutic hip joint injection.
The concern about steroid-induced cartilage effects and accelerated OA (Kompel 2019, McAlindon 2020 studies) is a real signal in the observational literature. The effect size is modest, causality is debated, and the practical implication is the now-standard recommendation to limit corticosteroid injection frequency to 3–4 per hip per year — not to avoid steroid injection altogether, which would deprive patients of a meaningful symptomatic tool.
Who Is a Good Candidate — and Who Isn’t
The strongest candidates for image-guided hip joint injection are: patients with symptomatic hip osteoarthritis (radiographically confirmed) whose pain has not responded to 6–12 weeks of physical therapy and conservative care; patients with femoroacetabular impingement and acetabular labral pathology in whom the hip joint’s contribution to the pain syndrome is uncertain (a diagnostic-plus-therapeutic injection both confirms the source and provides symptomatic relief); patients with inflammatory hip arthritis where the injection serves as a local adjunct to systemic disease-modifying therapy; patients who are not surgical candidates for hip replacement due to medical comorbidities, age, or personal preference; and patients who want to delay hip replacement while maintaining a level of function that supports work, exercise, and quality of life.
The procedure is not the right first-line treatment for: suspected septic hip arthritis (a surgical emergency); active skin infection over the injection site; pain that is primarily from the lumbar spine, the sacroiliac joint, or the trochanteric bursa (targeted workup of those structures is appropriate first); acute hip fracture; severe metallic implant artifact that precludes reliable image guidance; and patients on uncontrolled anticoagulation.
Comparison: Hip Injection vs. Other Hip Pain Treatments
Compared to oral anti-inflammatory medications and analgesics: NSAIDs and acetaminophen produce modest systemic pain reduction but carry cumulative gastrointestinal, cardiovascular, and renal risks; long-term opioids carry tolerance, dependence, and overdose risks. A single image-guided steroid injection produces more pain relief than sustained oral NSAID therapy in most patients and avoids the systemic exposure.
Compared to physical therapy alone: targeted physical therapy (hip abductor strengthening, core stabilization, hip internal rotation mobility work) is the foundational long-term management and should continue regardless of whether injections are performed. Injection and PT are complementary: the injection reduces pain to a level that enables productive PT, and the PT addresses the mechanical contributors that drive ongoing joint loading.
Compared to hyaluronic acid viscosupplementation: corticosteroid is faster-onset (3–7 days to meaningful relief vs. 2–4 weeks for HA), shorter-lasting (6–12 weeks vs. 3–6 months), more anti-inflammatory, and more consistently covered by insurance. HA is an alternative for patients who have responded to steroid but want longer intervals between injections or want to reduce cumulative steroid exposure. Some patients benefit from sequential trials of both.
Compared to platelet-rich plasma (PRP): PRP aims at biologic tissue support (growth factors to the cartilage and soft tissue) rather than inflammation reduction; has slower onset (4–8 weeks) and potentially longer duration (6–12 months); is generally self-pay; and has a weaker evidence base for hip OA than for tendinopathy. PRP is reasonable to discuss in patients with early-to-moderate hip OA who want to trial a biologic option.
Compared to hip arthroscopy: hip arthroscopy is a minimally invasive surgical procedure used to treat labral tears, cam-type femoral neck deformity in FAI, and loose bodies. It is appropriate for patients with mechanical symptoms (true catching, locking), significant FAI morphology on imaging, and failure of non-surgical options. Hip arthroscopy is not an alternative to injection — the two address different problems — but many arthroscopy candidates have also failed injection as part of the workup.
Compared to total hip arthroplasty (hip replacement): THA is the definitive surgical procedure for end-stage hip OA. It produces excellent pain relief and functional improvement with 90%+ 15-year implant survival, at the cost of surgical risk, a 6–12 week recovery, and a one-time procedure with finite implant lifespan. Image-guided hip injection is a non-surgical option appropriate for earlier disease, for patients who want to delay THA, and for patients who are not surgical candidates. The two are sequential, not competing, options.
What to Expect: The Patient Pathway
The full pathway from initial consultation to therapeutic hip injection at Modal Pain Management typically runs 2 to 4 weeks for a new patient.
Initial consultation visit (45 minutes). Dr. Movshis reviews your hip history, prior imaging, prior treatments, and medical context. A structured physical examination — including the FABER, FADIR, Stinchfield resisted flexion, Trendelenburg, and hip range-of-motion testing — confirms the hip as the pain source and rules out referred pain from the lumbar spine and SI joint. Imaging is reviewed. The diagnostic plan, the specific injectate (corticosteroid, HA, or PRP), expected response rates, alternatives, and cost/insurance picture are discussed in plain language.
Insurance authorization (5–10 business days). Our team submits prior authorization documenting conservative care, exam findings, and imaging.
Image-guided hip injection (15–25 minute procedure). Performed in our Midtown NYC office under live fluoroscopic or ultrasound guidance, with no IV sedation in most cases. You drive home after a 15–20 minute observation period.
Follow-up visit (15 minutes, 2–3 weeks after the injection). The pain diary is reviewed, the response objectively measured, and the long-term plan updated.
Ongoing management. Most patients combine intermittent injections with a sustained physical therapy program. When response shortens or disease progresses, the plan escalates to alternative injectates, to orthopedic surgical consultation, or (for patients with persistent post-arthroplasty pain) to peri-articular RFA techniques.
Recovery, Activity, and Return to Function
Recovery from image-guided hip injection is rapid. Post-procedure soreness at the injection site is common for 2–4 days and managed with ice and over-the-counter analgesics. A brief 1–3 day post-procedure pain flare before the steroid takes effect occurs in 5–10% of patients and is self-limited.
Most patients take the day of the procedure off, resume desk-based work the following day, and resume light walking the same evening. Activity guidance for the first 48 hours includes: avoiding high-impact loading (running, jumping, heavy lifting), avoiding prolonged standing, and avoiding activities that consistently reproduce the typical hip pain. Walking, stairs, and driving are permitted.
Full therapeutic effect is typically reached at 2–3 weeks. Many patients use the post-injection pain reduction as an opportunity to re-engage with physical therapy — particularly gluteus medius strengthening, which is the single best exercise intervention for mechanical hip pain and which is often difficult to sustain when pain is severe.
Insurance, Authorization, and Practical Logistics
Most commercial PPO plans cover image-guided corticosteroid hip joint injection when the clinical workup supports hip pathology and conservative care has been documented. Hyaluronic acid viscosupplementation for the hip is more variably covered. PRP is generally self-pay.
We accept most major commercial PPO plans (United Healthcare, Aetna, Cigna, BlueCross BlueShield, Oxford, Empire BCBS) and do not accept Medicare or Medicaid. We verify benefits and provide a written estimate before the procedure. Check accepted plans or call (646) 290-6660.
Why Patients Choose Modal Pain Management for Hip Injections
Dr. Alex Movshis is board-certified in Anesthesiology with subspecialty fellowship training in Interventional Pain Medicine, and performs all hip joint injections under live fluoroscopic or ultrasound guidance with contrast confirmation. We select the imaging modality and the injectate based on the individual clinical picture, the published evidence, and insurance coverage — corticosteroid for inflammatory and acute presentations, hyaluronic acid for patients seeking longer intervals and lower steroid exposure, PRP for patients interested in a biologic option with emerging evidence.
Our Midtown NYC office at 369 Lexington Avenue Floor 25 is one block from Grand Central Terminal. Same-week consultation appointments for new patients are typically available.
If you have groin or anterior thigh pain worse with weight-bearing and stairs, reduced hip range of motion, radiographic hip osteoarthritis that has not responded to conservative care, femoroacetabular impingement or a labral tear with uncertain symptomatic contribution, or persistent hip pain after physical therapy — image-guided hip joint injection may be the right next step. Learn more about the underlying conditions on our hip osteoarthritis and hip labral tear pages, or book a consultation to discuss whether you are a candidate.