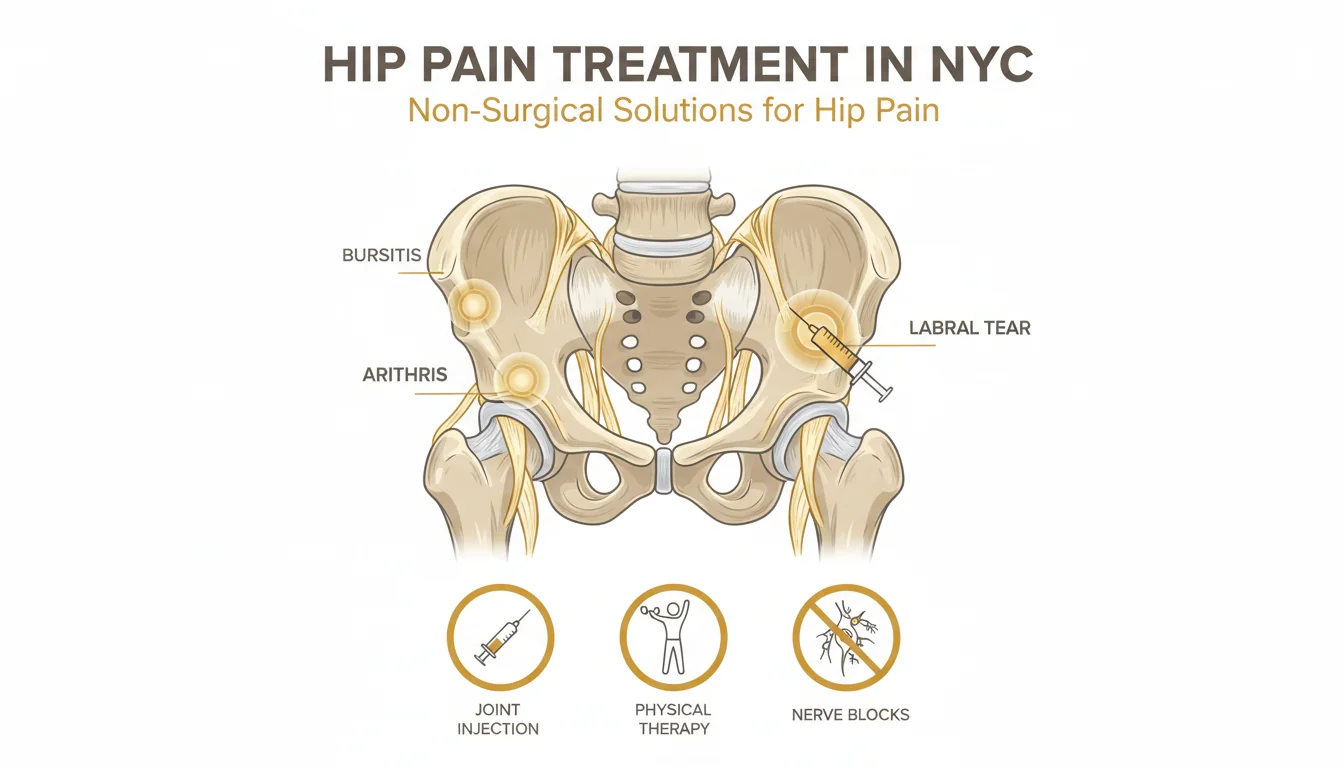
Hip labral tear and femoroacetabular impingement (FAI) are among the most common — and most frequently missed — causes of disabling deep groin pain in young and middle-aged adults. At Modal Pain Management in Midtown Manhattan, Dr. Alex Movshis uses high-resolution imaging, a focused physical examination, and image-guided diagnostic and therapeutic intra-articular hip injection to deliver a modern, structured non-operative pathway for labral tear and FAI — confirming the diagnosis, controlling the pain, retraining the mechanics, and reserving hip arthroscopy for the patients who actually need it.
This page covers what a hip labral tear actually is, why femoroacetabular impingement is usually the underlying mechanical driver, how labral tear is reliably distinguished from hip osteoarthritis and the other causes of groin pain, how Dr. Movshis diagnoses it, the evidence-based image-guided non-surgical treatment ladder we use, when hip arthroscopy is appropriate, and what to expect at your first visit.
Not Every Labral Tear Needs a Scope
The dominant clinical narrative around hip labral tears for the past two decades has been: MRI shows a labral tear, you get hip arthroscopy. The published evidence does not support that narrative for most patients. The landmark FASHIoN trial (Lancet, 2018) randomized patients with femoroacetabular impingement syndrome to hip arthroscopy versus a personalized non-operative hip therapy program — both arms improved, the surgical advantage at 12 months was modest (a 6.8-point difference on the iHOT-33 score), and a meaningful proportion of the non-operative group did not require surgery at extended follow-up. Independent cohort data and routine clinical experience confirm that many FAI/labral-tear patients managed with image-guided intra-articular injection, biologic injection (PRP), and targeted hip-stability physical therapy avoid surgery indefinitely.
This matters for two reasons. First, hip arthroscopy carries real risk — iatrogenic chondral injury, traction-related neuropraxia, heterotopic ossification, persistent groin pain in 10–20%, and a non-trivial conversion rate to total hip arthroplasty within 2–5 years in patients with pre-existing chondral wear or borderline dysplasia. Second, asymptomatic labral tears are extremely common — autopsy and asymptomatic-volunteer MRI studies consistently show labral abnormalities in 50–69% of asymptomatic adults — so a labral tear on MRI is not, by itself, a surgical indication. The clinical question is not “is there a tear?” — it is “is the hip joint generating the pain, what mechanical factors are driving it, and what structured treatment will restore function?”
Modal Pain Management’s role in this is to deliver the structured non-operative pathway with the same precision a hip arthroscopist applies in the operating room — image-guided diagnostic injection, image-guided therapeutic injection, biologic injection where indicated, and articular branch radiofrequency ablation for refractory cases — and to refer to one of the strong NYC-based hip arthroscopy programs when surgery is genuinely the right answer.
Why It Hurts There: The Anatomy of Labral Tear and FAI
The hip is a ball-and-socket synovial joint. The femoral head sits in the acetabulum (the cup of the pelvis), and the rim of the acetabulum is encircled by the acetabular labrum — a triangular fibrocartilaginous ring that deepens the socket, increases joint stability, and seals synovial fluid into the joint to maintain hydraulic pressure across the articular surfaces. The labrum is innervated by free nerve endings, particularly in its anterosuperior portion, which is why labral tearing produces pain. Its blood supply, however, is limited to the peripheral one-third — the inner two-thirds are largely avascular and do not heal back to native tissue once torn.
In femoroacetabular impingement (FAI), abnormal bony morphology causes premature contact between the femoral head-neck junction and the acetabular rim during routine hip motion. Cam impingement is an aspherical, non-round femoral head-neck junction (typically anterolateral) that bumps into the acetabular rim during hip flexion and internal rotation, shearing the labrum and the adjacent chondral surface from the bone. Pincer impingement is overcoverage of the femoral head by an abnormally deep or retroverted acetabulum, with the acetabular rim crushing the labrum on flexion. Most symptomatic patients have mixed cam-pincer impingement. The labral tear is a downstream consequence of the impingement mechanics — which is why surgical labral repair without correcting the underlying bony morphology has historically failed, and why a targeted motor-control and hip-stability physical therapy program (which alters how the hip moves through the impinging arc) is one of the most evidence-based non-operative treatments.
Pain in labral tear and FAI is generated by multiple structures: the torn labrum itself (free nerve endings in its anterosuperior portion), the irritated joint capsule, the inflamed synovium that develops in response to the chondral and labral injury, and the articular branches of the femoral and obturator nerves that innervate the anterior hip capsule. This last point is clinically important: image-guided intra-articular injection delivers medication directly to the synovium, capsule, and labrum simultaneously, and image-guided radiofrequency ablation of the femoral and obturator articular branches denervates the painful capsule for refractory cases — both interventions exploit the multi-source pain anatomy that a labral repair alone does not address.
Understanding this anatomy explains why image-guided treatment matters. The intra-articular space is small and surrounded by major neurovascular structures (femoral artery and vein, femoral nerve, sciatic nerve). Blind landmark injection into the hip joint has published accuracy of only 50–65%, while fluoroscopic or ultrasound-guided injection is consistently >90% accurate. Treatment delivered into the wrong tissue does not work.
Hip Labral Tear vs. The Other Causes of Hip and Groin Pain
The single most important step in evaluating hip and groin pain is determining where the pain actually is and what is generating it. The differential diagnosis is wide and the wrong diagnosis leads to the wrong treatment.
Hip labral tear and FAI typically produce deep anterior groin pain, mechanical and intermittent (worse with hip flexion, twisting, prolonged sitting, deep squat), often with mechanical symptoms (clicking, catching, snapping, or transient locking), positive FADIR test on physical exam, and most commonly in patients in their 20s–40s with a history of high-volume hip flexion sport. The C-sign — patients cupping the front of the hip in a C-shape — is classic.
Hip osteoarthritis typically produces deep anterior groin pain similar in location to FAI but with a more constant, mechanical (load-related) pattern, prolonged morning stiffness (15–60 minutes), restricted internal rotation on exam, and X-ray findings of joint space narrowing and osteophytes. Most common in patients over 50. Coexisting FAI and OA is common — a labral tear in the setting of advanced OA (Tönnis grade 2+) is treated very differently from an isolated labral tear in a 30-year-old.
Greater trochanteric pain syndrome (hip bursitis / GTPS) produces lateral hip pain over the bony prominence on the outside of the upper thigh, worse lying on the affected side at night, with tenderness on direct palpation. This is gluteus medius and minimus tendinopathy with secondary bursal inflammation — Modal Pain Management treats it on a separate page.
Sacroiliac (SI) joint dysfunction produces deep buttock pain just inferior and medial to the dimples of Venus (the Fortin finger sign), worse with single-leg standing and asymmetric loading, with positive provocative tests (FABER, distraction, compression, thigh thrust). Frequently mislabeled as lumbar disc or hip pain.
Piriformis syndrome produces deep buttock pain that worsens with prolonged sitting and may radiate down the back of the leg, mimicking sciatica. Reproduced by the FAIR test.
Athletic pubalgia (“sports hernia”) produces lower abdominal and adductor-region pain with kicking, cutting, and sit-ups, in athletes (soccer, ice hockey). Frequently coexists with FAI in elite athletes — the dual pathology must be recognized to avoid treating only half the problem.
Adductor strain / tendinopathy produces pain along the adductor longus tendon at the pubic symphysis, reproduced by resisted adduction, more localized than intra-articular hip pain.
Iliopsoas tendinopathy / snapping hip (internal coxa saltans) produces an audible or palpable snap at the front of the hip with hip flexion-extension, often with anterior groin discomfort, and may coexist with intra-articular pathology.
Lumbar radiculopathy (L1–L2) can produce groin pain referred from the upper lumbar nerve roots — usually with a history of low back pain and reproduction of symptoms by lumbar maneuvers.
Femoral neck stress fracture in runners, military recruits, and patients with low bone density — groin pain that worsens progressively with running, with pain on hop test or single-leg stance. A diagnosis not to miss; MRI is required.
Avascular necrosis (osteonecrosis) of the femoral head produces deep groin pain often without injury, particularly in patients with chronic corticosteroid use, sickle cell disease, heavy alcohol use, or after a hip fracture or dislocation. MRI is required for early diagnosis before subchondral collapse.
A focused history and physical examination at the consultation visit narrows this list to 1–2 leading possibilities; imaging and, when needed, image-guided diagnostic intra-articular injection then confirms the pain generator before any therapeutic intervention is performed.
How Hip Labral Tear Is Diagnosed
Diagnosis combines history, physical exam, imaging, and — when the picture is incomplete — diagnostic image-guided intra-articular injection.
History looks for the characteristic mechanical pattern: deep anterior groin pain in a young or middle-aged adult, provoked by hip flexion (sitting in a low chair, deep squatting, prolonged car or airline travel) and by twisting or pivoting, often with mechanical symptoms (clicking, catching, locking, or giving way). A history of high-volume hip flexion sport (soccer, ice hockey, dance, gymnastics, martial arts, CrossFit, golf) raises pre-test probability. Sudden onset after a specific injury — a fall onto the hip, a sudden cutting maneuver, a hip dislocation — is also common.
Physical exam focuses on provocative maneuvers that compress the labrum and the femoral head against the acetabular rim. The FADIR test (passive flexion, adduction, and internal rotation of the hip) is the most useful single test — sensitivity of 80–90% for intra-articular hip pathology — and reproduces the patient’s deep groin pain. The FABER test (figure-of-four position) is positive in both intra-articular hip pathology and SI joint dysfunction. The scour test and resisted straight-leg raise can also reproduce intra-articular pain. Range of motion is examined for the loss of internal rotation that suggests cam impingement and for the loss of flexion that suggests pincer impingement. A neurologic exam excludes lumbar radiculopathy, and the lateral hip is palpated to rule out greater trochanteric pain syndrome.
Plain radiographs are obtained first and include a standing anteroposterior pelvis view and a lateral view of the affected hip (Dunn lateral or frog-leg). The plain films are inspected for cam morphology (an aspherical femoral head-neck junction; alpha angle >55°), pincer morphology (a deep or retroverted acetabulum; lateral center-edge angle >40°, crossover sign), joint space narrowing (suggesting coexisting osteoarthritis and changing the treatment calculus), borderline dysplasia (lateral center-edge angle <25°, which contraindicates many arthroscopic procedures), and other diagnoses (femoral neck stress fracture, avascular necrosis with subchondral collapse).
Magnetic resonance arthrography (MRA) — MRI performed after intra-articular injection of dilute gadolinium contrast — is the imaging gold standard for labral tear, with reported sensitivity of 87–95% versus 30–66% for non-contrast MRI. The intra-articular contrast distends the joint and outlines labral pathology that conventional MRI sequences miss. MRA also detects associated chondral injury, paralabral cysts, ligamentum teres injury, and (importantly) coexisting osteoarthritis. Modern 3T non-contrast MRI with dedicated hip protocols closes some of this sensitivity gap and is reasonable when MRA is not available.
Image-guided diagnostic intra-articular hip injection serves as a final diagnostic step when imaging is equivocal or when there are multiple potential pain generators (frequently FAI/labral coexisting with SI joint or trochanteric pathology). Fluoroscopic or ultrasound-guided injection of local anesthetic (typically with corticosteroid for therapeutic effect) is performed in the office; substantial pain relief in the first 1–2 hours after injection (the diagnostic anesthetic phase) confirms that the hip joint itself is generating the pain and predicts a favorable response to therapeutic intervention. This diagnostic injection is one of the most useful tests in hip pain workup and is frequently the step that separates “labral tear that needs treatment” from “labral tear that is an incidental MRI finding.”
The Image-Guided Non-Surgical Treatment Ladder
Modal Pain Management uses a structured, evidence-based, image-guided treatment ladder for hip labral tear and FAI. The ladder is sequenced — most patients work through the early steps before considering arthroscopy — and the treatments are designed to address the multiple pain generators (synovitis, capsular irritation, articular nerve sensitization, abnormal mechanics) rather than only the structural tear.
Step 1: Image-guided diagnostic and therapeutic intra-articular injection. Fluoroscopic or ultrasound-guided injection of local anesthetic plus corticosteroid serves a dual purpose. The anesthetic phase confirms (or excludes) the hip joint as the pain generator within hours of the injection. The corticosteroid phase quiets the synovitis and capsular inflammation and produces 6–12 weeks of pain control in 70–80% of patients with appropriately diagnosed intra-articular hip pathology. This window of pain control is what makes productive physical therapy possible — patients who could not engage in motor-control work because of pain can now retrain the mechanics that drive the impingement.
Step 2: Targeted hip-stability and motor-control physical therapy. This is the single most evidence-based non-operative treatment for FAI/labral tear and the most common reason patients improve without surgery. The program — delivered by a physical therapist with specific hip-stability expertise — focuses on gluteus medius and minimus strengthening, deep hip external rotator activation, lumbopelvic motor control, hip flexor length and quality, and sport- or work-specific movement retraining. The goal is to alter how the hip moves through the impinging arc — for example, reducing the anterior pelvic tilt that increases impingement during squatting and reducing the femoral internal rotation moment during gait. A typical program runs 8–12 weeks. The FASHIoN trial used a structured hip therapy program closely modeled on this approach.
Step 3: Platelet-rich plasma (PRP) intra-articular injection. Image-guided autologous PRP delivers concentrated platelets and their growth factors (PDGF, TGF-β, VEGF, IGF-1) directly to the labrum, capsule, and chondral surface. The mechanism of action is biologic support of the synovium and chondral surface and modulation of the inflammatory environment in the joint, rather than re-growing labral tissue. Emerging evidence — including head-to-head studies comparing PRP with hyaluronic acid in mild-to-moderate hip pathology — shows PRP produces medium-term durable pain relief in suitable candidates, and the safety profile is excellent because the product is autologous. PRP is most useful for patients in their 20s–40s with mild-to-moderate intra-articular pathology who want to delay or avoid arthroscopy.
Step 4: Hyaluronic acid (viscosupplementation) intra-articular injection. Hyaluronic acid is FDA-approved for the knee and used off-label in the hip. The mechanism is restoration of the viscoelastic properties of the synovial fluid, improvement in joint lubrication, and modulation of synovial inflammation. Evidence in the hip is mixed but a substantial subset of patients gets 4–6 months of relief, and the agent is particularly useful in patients with concurrent early osteoarthritis where corticosteroid is undesirable.
Step 5: Image-guided radiofrequency ablation (RFA) of the articular branches of the femoral and obturator nerves. The anterior hip capsule is innervated by the articular branches of the femoral nerve (laterally) and the obturator nerve (medially). For patients with refractory hip pain who are not surgical candidates or who want to delay arthroscopy, image-guided RFA of these articular branches denervates the painful capsule and produces 6–12 months of pain relief. Modal Pain Management performs articular branch RFA under fluoroscopic or ultrasound guidance with a diagnostic block first to confirm response. This is the genicular-RFA-equivalent for the hip and has become an important tool in the modern hip-preservation playbook.
Step 6: Hip arthroscopy referral. When non-operative care has been completed and pain or mechanical symptoms persist, hip arthroscopy is the appropriate next step. The procedure typically combines acetabular rim trimming (for pincer), femoral head-neck osteochondroplasty (for cam), and labral repair or selective debridement. Modal Pain Management refers to NYC-based hip arthroscopists for patients who meet appropriate criteria: imaging-confirmed structurally significant FAI; true mechanical symptoms (locking, catching, giving way) caused by an unstable labral flap or loose body; high-level athletic or occupational demand; and failure of 3–6 months of structured non-operative care. Patients with advanced osteoarthritis (Tönnis grade 2+), borderline or frank dysplasia, or age >50 with normal hip morphology are typically poor arthroscopy candidates — for those patients, the right pathway may be continued non-operative care or, ultimately, total hip arthroplasty.
Physical Therapy and Self-Care for Labral Tear and FAI
Several patient-controlled measures have a measurable effect on labral tear and FAI symptoms and are part of every treatment plan.
Activity modification reduces the symptomatic flares without eliminating activity. Specific modifications: avoid prolonged deep hip flexion (low chairs, deep car seats, long airline flights without aisle breaks), avoid repetitive cutting and pivoting sports during a flare, replace deep squats with box squats or partial-range squats during physical therapy, and avoid the specific provocative motion that reproduces the patient’s symptoms (often hip flexion plus internal rotation).
Hip-stability strengthening — gluteus medius, gluteus minimus, deep hip external rotators, and core/lumbopelvic motor control — directly alters how the hip moves through the impinging arc and is the most evidence-based single intervention for FAI. A typical program runs 8–12 weeks under a physical therapist with hip expertise.
Hip flexor length and quality work — focused on iliopsoas and rectus femoris — relieves anterior hip tightness that worsens impingement during sitting and standing. A short daily program of hip flexor mobilization (couch stretch, half-kneeling stretch, active hip extension) is standard.
Cycling, swimming, and aquatic exercise are excellent low-impact alternatives to running and high-impact sport during a flare and during the early phase of physical therapy. Stationary cycling with appropriate seat height (high enough to avoid deep hip flexion at the top of the stroke) maintains aerobic fitness without provoking the impinging arc.
Weight management reduces hip joint load — every pound of body weight produces approximately 3–6 pounds of force across the hip joint during walking, and modest weight loss (5–10% of body weight) produces measurable reductions in pain.
Sleep posture matters: sleeping on the affected side without a pillow between the knees crowds the hip in adduction and aggravates symptoms. A pillow between the knees in side-lying, or supine sleep, is preferred during a flare.
When Hip Pain Is an Emergency
Most hip pain — including FAI and labral tear — is not an emergency and is appropriately worked up in the outpatient setting. Several presentations are different and require urgent evaluation rather than an outpatient pain management visit.
Severe hip pain with fever, chills, or systemic illness raises concern for septic arthritis — particularly in patients with diabetes, recent joint procedure, immunosuppression, or IV drug use. Septic arthritis is a surgical emergency.
Severe hip pain after trauma, particularly the inability to bear weight, raises concern for hip fracture or hip dislocation and requires immediate emergency evaluation. In older adults, falls from standing height can produce occult femoral neck fracture that requires CT or MRI to identify.
New, severe groin pain in a patient with sickle cell disease, chronic high-dose corticosteroid exposure, heavy alcohol use, organ transplant history, or prior hip fracture or dislocation raises concern for avascular necrosis (osteonecrosis) of the femoral head — early diagnosis on MRI before subchondral collapse changes the surgical options dramatically.
Progressive groin pain in a runner, military recruit, or patient with low bone density raises concern for femoral neck stress fracture — a diagnosis not to miss because completed fractures of the femoral neck have a high rate of avascular necrosis. A dedicated MRI is required.
New hip pain in a patient with a history of cancer raises concern for metastatic disease and requires imaging.
If any of these red flags are present, the right next step is the emergency department or a same-day orthopedic evaluation, not an outpatient pain management consultation.
Why Modal Pain Management
Modal Pain Management is a Midtown Manhattan pain management practice (369 Lexington Avenue) led by Dr. Alex Movshis, a board-certified pain management physician with subspecialty training in interventional pain medicine and image-guided procedures. The practice was built around a small set of organizing principles that matter for hip labral tear and FAI: every diagnostic injection and every therapeutic injection is performed under fluoroscopic or ultrasound guidance (no blind injections); the diagnostic process is structured to confirm the actual pain generator before any therapeutic intervention is performed (because labral tears on MRI are extremely common in asymptomatic adults); the treatment ladder is evidence-based and sequenced from least to most invasive (image-guided injection, biologic injection, articular branch RFA, surgical referral); and surgical referral is offered honestly when arthroscopy is the right answer rather than reflexively or never. Modal Pain Management works directly with NYC-based hip arthroscopists and orthopedic surgeons and the consultation visit produces a clear written treatment plan within 45 minutes — most patients leave knowing exactly what their next step is. Most major insurance is accepted, and same-week appointments are typically available.